Acute Laryngitis
Introduction:
Larynx because of its position i.e. anterior to the aero digestive tract is vulnerable to various insults. These insults cause inflammation of larynx. These insults could be infective and non infective.
Definition: Acute laryngitis is a inflammatory condition that affects the vocal cords and supraglottis.
Etiology:
1. Upper respiratory tract infections
2. Rarely neck space infections / parapharyngeal abscess / retropharyngeal abscess can cause acute laryngitis
3. Gastro-oesophageal reflux disease (GERD) can cause posterior glottic and arytenoid infection
4. Non-specific inflammation like sarcoidosis / Wegner's granulomatosis can also cause laryngitis
5. Allergy
6. Inhalation of dusts / fumes
Pathophysiology: Moraxella catarrhalis infections have been attributed. Patients with acute laryngitis show early glottic contact at the mid portion of the mebranous cord.
Clinical features:
1. Change / loss of voice
2. Sore throat and otalgia
3. Difficult / painful swallow
4. Tender larynx with or without cervical adenopathy
5. Difficulty in breathing / stridor (rare)
Voice in acute laryngitis: Voice in laryngeal infections are usually weak, breathy, rough. Rerely there may be aphonia.
If stridor is present it could be inspiratory due to narrowing of supra glottis or glottis. Expiratory stridor is caused due to narrowing of subglottis.
Indirect laryngoscopy shows:
1. Inflammation and swelling of supraglottis, glottis and subglottis. Vocal cords may appear reddish and oedematous.
2. There may be pooling of saliva in the hypopharynx if there is associated odynophagia.
Management:
Resolves completely within 10 days in most cases. Therapy includes complete voice rest, avoidance of irritants and steam.
Antibiotics are reserved for severe forms of laryngitis (Bacterial). Since the common pathogen is Moraxella catarrhalis Erythromycin is the drug of choice.
In case of residual speech disturbances speech therapy is indicated.
Acute epiglottitis: This condition is also known as supraglottitis. This condition affects the epiglottis primarily, but other adjacent sites like lingual tonsil, aryepiglottic folds and false cords are also affected. Epiglottitis affects all age groups. In children it could progress rather rapidly leading on to airway compromise. This feature is rather uncommon in adults. Hemophilus influenza is the common causative organism.
Clinical features: Drooling, respiratory distress, painful swallowing, change in voice.
Examination will show inflammed epiglottis, aryepiglottic folds, and arytenoid cartilages. These patients also commonly have cervical adenopathy.
Plain x-ray soft tissue of neck shows enlarged epiglottis ("Thumb sign"), and absence of deep well defined vallecula ("Vallecula sign").
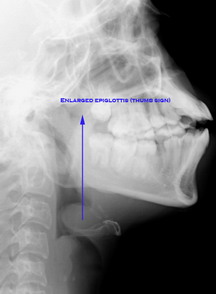
Xray neck showing Thumb sign
Complications:
1. Respiratory distress
2. Epiglottic abscess
3. Internal jugular vein thrombosis
Management:
These patients should be admitted for observation.
Airway obstruction if any should be tackled by emergency tracheostomy.
Antibiotics of choice include third generation cephalosporins.
Croup (Laryngotracheobronchitis):
The work "croup" is scottish. It denotes sore throat with hoarse breathing. This disease commonly affects small children (age group 6 months - 3 years). These children have subglottis oedema, which leads to respiratory distress and biphasic stridor. Croup is uncommon in adults.
Etiology: Laryngotracheobronchitis is usually caused by viral infection. Paromyxovirus, para influenza virus Types I and II have been implicated.
In adults Herpes simplex has been implicated.
This form of laryngitis is characterised by subglottic oedema. The reason for involvement of subglottis mucosa is still unknown.
Clinical features:
1. Cough
2. Sore throat
3. Malaise
4. Mild fever
5. Stridor (inspiratory)
Endoscopy shows:
Normal epiglottis, inflammed vocal cords and subglottic oedema which extends to trachea.
Management:
Oxygenation
Steroids
Broad spectrum antibiotics ( to prevent secondary infections)
Pertussis: (Whooping cough):
This acute illness is caused by Bordetella pertussis. This disease affects patients of all age groups. Bordetella pertussis produces endotoxin and exotoxins which destroys cilia and stops the bronchial epithelium from functioning. This condition is most severe in children. Adults have a less severe disease. Immunisation has reduced the incidence of this disease.
Clinical features:
These patients present with runny nose, dry cough, and mild fever. This condition may mimic common cold. Cough occurs in paroxysms and is followed by gasping and the characteristic whoop in children.
Diagnosis:
Is confirmed by serology, nasopharyngeal aspirate culture and PCR reaction.
Management:
7 - 14 day course of erythromycin is recommended.
