Blow out Fracture
Introduction: Orbital fractures commonly occur in maxillo facial trauma causing enophthalmos and diplopia. If not properly managed the cosmetic and functional problems can virtually become intreatable. In recent years management of these fractures have been virtually standardized with special emphasis on fixation of fractured fragments and exact anatomical approximation.
Definition: Blow out fracture is defined as a clinical syndrome in which there is fracture of orbital walls with intact rim. When rim is not involved it is known as pure orbital blow out fracture. If orbital walls and rims are also involved in the fracture then it is known as impure orbital blow out fracture.
History: Blow out fracture of orbit was first described by Lang in early 1900's. The exact description of the fracture and the terminology (blow out fracture) was first coined by Converse and Smith. It was infact Smith who first described inferior rectus entrapment in between the fractured fragments, causing decreased ocular mobility.
Classification of blow out fractures:
. Orbito zygomatic
. Naso - Orbito - Ethmoid (NOE)
. Internal blow out
. Complex ( Any of the above combinations)
The type of fracture sustained depends on the amount of force and the direction of force which caused the injury.
Etiology: Orbital fractures are commonly caused by road traffic accidents. Pure blow out fractures involving the orbit are sustained by impact injuries to orbit and upper eyelid caused by an object which is fairly large enough to cause fracture and does not penetrate the orbit. These types of injuries are common in boxers, base ball players, cricket players etc.
Theories accounting for blow out fracture: The exact mechanism causing blow out fracture is yet to be elucidated. Two theories have been going around for quite sometime. They are:
1. Buckling theory
2. Hydraulic theory
Buckling theory: This theory proposed that if a force strikes at any part of the orbital rim, these forces gets transeferred to the paper thin weak walls of the orbit (i.e. floor and medial wall) via rippling effect causing them to distort and eventually to fracture. This mechanism was first described by Lefort.
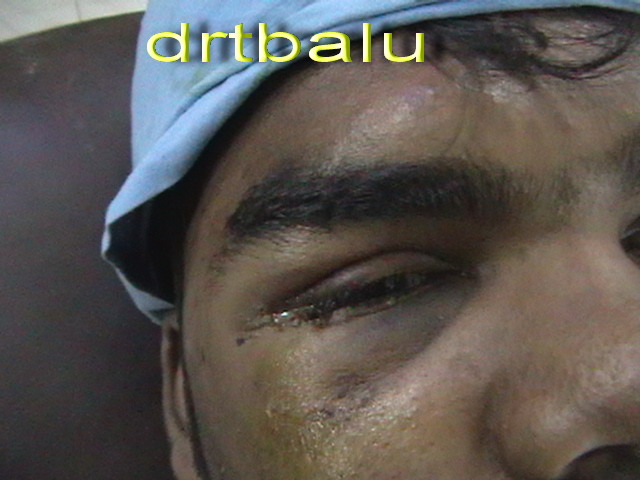
Clinical photograph of a patient with blow out fracture
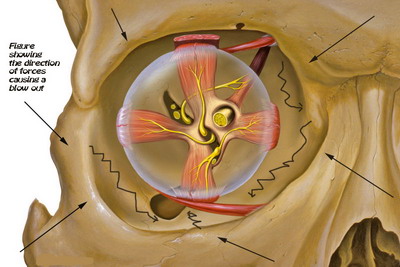
Figure showing the direction of forces via the rippling effect accounting for the Buckling theory
Hydraulic theory: This theory was proposed by Pfeiffer in 1943. This theory believes that for blow out fracture to occur the blow should be received by the eye ball and the force should be transmitted to the walls of the orbit via hydraulic effect. So according to this theory for blow out fracture to occur the eye ball should sustain direct blow pushing it into the orbit.
Water House in 1999 did a detailed study of these two mechanisms by applying force to the cadaveric orbit. He infact used fresh unfixed cadavers for the investigation. He described two types of fractures:
Type I: A small fracture confined to the floor of the orbit (actually mid medial floor) with herniation of orbital contents in to the maxillary sinus. This fracture was produced when force was applied directly to the globe (Hydraulic theory).
Type II: A large fracture involving the floor and medial wall with herniation of orbital contents. This type of fracture was caused by force applied to the orbital rim (Buckling theory).
Clinical features of blow out fracture:
. Intraocular pain
. Numbeness of certain regions of face
. Diplopia
. Inability to move the eye
. Blindness
. Epistaxis
Patient may also show signs of:
. Enophthalmos
. Oedema
. Haematoma
. Globe displacement
. Restricted ocular mobility
. Infraorbital anesthesia
Proptosis in these patients is sinister because it indicates retrobulbar / peribubar hemorrhage.
Pupillary dysfunction associated with visual disturbances indicate injury to optic nerve and it is an emergency. Patient must be taken up for immediate optic nerve decompression to save vision.
A complete ophthalmic examination is a must in all these patients.
Indications for operative repair:
1. Diplopia within 30 degrees of primary gaze
2. Extraocular muscle entrapment
3. Enophthalmos greater than 2mm
Applied anatomy:
In adults the orbital floor is contributed by maxillary, zygomatic and palatine bones. It is infact the shortest of all the orbital walls. It does not reach up to the orbital apex, but terminates at the level of posterior edge of maxillary sinus. It is infact the weakest portion of the orbital walls made still more weak by the infra orbital groove.
Investigations:
X -ray paranasal sinuses: May show the classical "tear drop sign" of prolapsed orbital contents. The fractured fragment may also be visible. The corresponding maxillary sinus may appear hazy due to the presence of hemosinus.
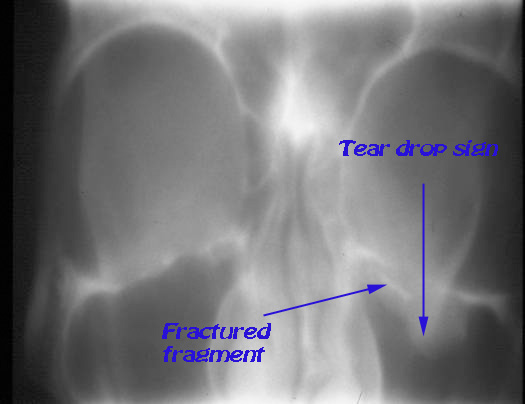
X-ray PNS showing tear drop sign
CT scan:
This is virtually diagnostic.
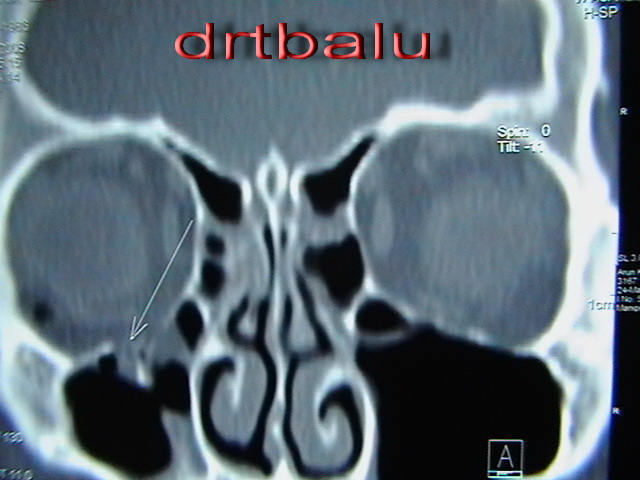
Coronal CT image of nose and sinuses showing features of Blow out fracture
Timing for surgical intervention:
This is highly controversial. Some of the authors prefer a waiting period of atleast 2 weeks for the oedema to resolve before proceeding with surgical reduction of the fracture. Early intervention is indicated only in white eyed blow out fracture which is common in children. In children the bones are flexible and does not break easily but bends. Significant amounts of orbital tissue may get entrapped in between the fractured fragments causing a compromise in their blood supply. This condition is known as the white eyed blow out fracture. These patients should under go immediate reduction.
Surgery:
The main aim of surgery is open reduction and fixation of the fractured fragments.
The main support for the anterior projection of eye ball comes from the posterio medial and posterio lateral walls of the orbit. These areas diverge like a fan / cupped hand holding the globe forwards. Both these walls are paper thin and are commonly damaged in blow out fractures. It has been clinically shown that repair is easy if these supporting walls are intact. If this key area is involved, it should be reconstructed first.
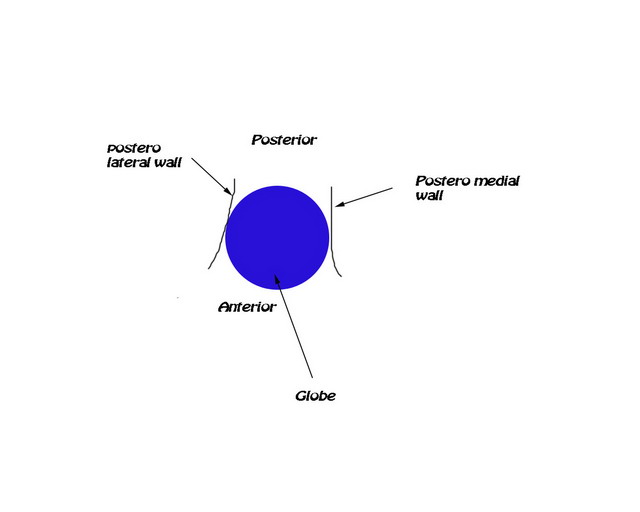
Diagram showing support to the orbit
Surgical access to the floor of the orbit:
Orbital floor can be accessed by any of the following incisions:
1. Subciliary / lower blepharoplasty
2. 2nd crease / subtarsal
3. Transconjunctival
The major advantage of these incision is that it is cosmetically acceptable. There is also no risk of lower eyelid shortening or inversion.
Subciliary incisions are made 2mm below the edge of the eye lid. Midtarsal incision is sited between the edge of the eyelid and the orbital rim.
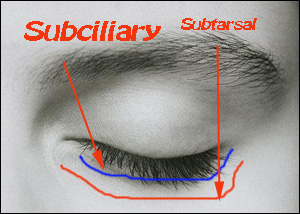
Diagram showing various incisions used to access the orbital floor
The incision is made through skin only. The skin is reflected down by blunt dissection until it is free from the pretarsal portion of the orbicularis oculi muscle. The muscle fibers of orbicularis oculi are spread to expose the periosteum of the lateral border initially. The submuscular dissection is continued till the orbital septum is seen. Care must be taken not to incise / damage the orbital septum as it can cause troublesome prolapse of orbital fat. Damage to orbital septum can also lead to lower eye lid shortening.
Infra orbital rim is now identified. Periosteum is incised and the prolapsed contents of the orbit is elevated to visualise the floor of the orbit. The fracture can now be visualised. It can be reduced and immobilised using micro plates and screws.
Transconjunctival method: Was popularised by Tessier. This procedure does not involve any disruption to the outer surface of the eyelid.
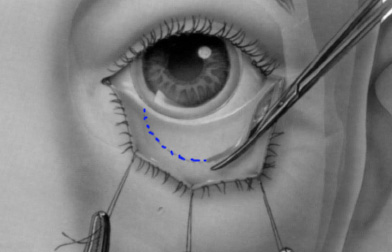
Incision for transconjunctival approach
In this method the lower eye lid is pulled forward. To increase the laxity a lateral canthotomy should be performed.
Two methods can be performed via this incision. 1. Preseptal method and 2. Retroseptal method.
Preseptal method: In this method incision is made at the edge of the tarsal plate to create a space infront of the orbital plate to reach the orbital rim.
Retroseptal method: In this method an incision is sited 2mm below the tarsal plate to reach the orbital rim.
The major advantage of this procedure is there is virtually very minimal scar formation. It is very quick to perform and involves no skin, muscle dissection. The only disadvantage is the limitation of access to the medial portion of the orbital floor.
In cases of blow out fractures involving the medial portion of the floor of the orbit Caldwel luc procedure can be performed to reduce the fracture fragment. Nasal endoscope can be introduced through the caldwel luc fenestra to improve visualisation.
Reconstruction materials:
In cases of extensive destruction of the floor of orbit then reconstruction of the floor must be resorted to using implants. These materials include autologous bone grafts and titanium plates / meshes.
