CSF Rhinorrhoea
Definition: CSF discharging from the nose is known as CSF rhinorrhoea. Cerebrospinal fluid is a clear colorless fluid that bathes the brain and spinal cord, cushioning them against trauma. In fact in literal terms the brain and spinal cord floats in the cerebrospinal fluid. The specific gravity of brain is only 4% of that of CSF, hence it could float easily in the CSF.
Functions of CSF:
1. It cushions the brain and spinal cord against trauma.
2. It nourishes the brain tissue.
3. It removes waste materials.
Anatomy:
The brain and spinal cord is covered by 3 layers of meninges: They are 1. The duramater
2. Piamater
3. Arachnoid
These layers of meninges bound three spaces between them. They are:
1. Epidural space: is the space that lies between the inner perioseteal lining of the skull / vertebral canal and the duramater.
2. Subdural space: is the space that lie between the duramater and the arachnoid.
3. Subarachnoid space: lies between arachnoid and piamater. This space contains the cerebrospinal fluid. This space continues with the ventricles of the brain. Large blood vessels of the brain traverse this space. This space also extends along the olfactory nerves to the mucoperiosteum of the nasal cavity. It also extends along blood vessels as they enter and exit the brain. At its inferior aspect the subarachnoid space is dilated and becomes lumbar cistern. This area is accessed while doing a lumbar puncture.
Figure showing anatomy of Meninges
Ventricles: are 4 CSF filled cavities in the brain. These ventricles are lined by ependyma (cuboidal epithelium). This lining has a secretory function.
Lateral ventricles: are two in number one in each cerebral hemisphere. These lateral ventricles communicate with the Foramen of Munroe to the third ventricle. Choroid plexus of the lateral ventricle are located in the medial wall of the ventricle.
3rd and 4th ventricles: are unpaired, midline ventricles. The third ventricle is connected to the lateral ventricles by the Foramen of Munroe. The third and the fourth ventricles are connected to each other by the Aqueduct of Sylvius. This aqueduct is lined by ependyma and does not contain choroid tissue. The choroid plexus of the third ventricle is found over the roof.
The third ventricle is a slit like cleft lying between the thalami of the brain. The fourth ventricle is situated anterior to cerebellum and posterior to the pons. The fourth ventricle continues inferiorly with the central canal of the spinal cord.
These ventricles communicate with the subarachnoid space through 3 openings in the roof of the 4th ventricle. They are 1. Foramen of Magendie, which is a single foramen located over the roof of the 4th ventricle and 2. Foramen of Luschka which are 2 in number present laterally.
Physiology of CSF circulation:
The normal CSF pressure ranges between 60 - 150 mm of water. This pressure varies according to age, position of the head and other associated factors. It is increased during valsalva manuvers, coughing and straining. It is also increased during jugular vein compression.
CSF pressure in neonates is very low due to the pliability of the cranial cavity prior to the closure of cranial sutures.
CSF production: The choroid plexus located inthe lateral 3rd and 4th ventricles produces CSF. This accounts for 2/3 of the total production. Extra choroidal production occurs in the ependyma tissue of the ventricle. The rate of production of CSF is about 500 cc / day, or 0.30ml/min. In adults the total CSF volume is 150ml. The whole volume of the CSF is turned over about 3 times a day.
CSF absorption: Occurs at the arachnoid villi and arachnoid granulation. These are finger like projections intimately associated with the dural venous sinus. Resorption is a passive phenomenon, obeying the laws of pressure gradiant.
Figure showing lateral view of ventricles and CSF circulation
CSF flows from the site of production in the ventricles through the foramen of Megendie and Luschka exiting the cisterna magna and the basal cisterns to enter the subarachnoid space. The arterial pulsations propels the CSF from the ventricles into the subarachnoid spaces overlying central convexities. Flow within the spinal cord is facilitated by motions of the vertebral column.
CSF Leaks always occur when the barrier that retains the Cerebrospinal fluid is breached. These barriers are skin, galeal periosteum, skull, dura and arachnoid. The mucosal lining of the nasal cavity also forms its last line of defence.
Causes of CSF rhinorrhoea:
Traumatic:
a. Accidental: Acute / Delayed
b. Iatrogenic: Acute / Delayed
Non traumatic:
a. High pressure
i. Tumors: Direct / Indirect
ii. Hydrocephalus
b. Normal pressure:
i. congenital anamolies
ii. Focal atrophy - Olfactory / Sellar
iii. Osteomyelitic erosion
iv. Idiopathic
Types of CSF rhinorrhoea:
I. Traumatic
II. Non traumatic (spontaneous) - a. High pressure leaks (always associated with concommitant hydrocephalus)
The high pressure leaks are commonly encountered in the cribriform area. This is due to the fagility and unique anatomy in this area i.e. (prolongation of the subarachnoid space along the olfactory filaments). The leak during these conditions functions as a safety valve alleviating the increased intracranial pressure. These high pressure leaks are associated with slow growing tumors and 1/4 of them have hydrocephalus. Pituitary neoplasms are the most common type of intracranial tumor found, next common are the posterior cranial fossa lesions. Direct invasion of the skull base is not the usual mechanism of this leak. Closure of these leaks may worsen the condition of the patient if the causative lesion is left untreated.
b. Normal pressure leaks - These leaks are associated with congenital dehiscence or thin bone along the skull base. Commonly this type of leaks occur in the ethmoidal sinus adjacent to the cribriform plate. Potential leak pathways include the prolongation of the subarachnoid space along the olfactory nerves and stalk of the hypophysis. Minor degrees of maldevelopment of the cribriform plate or the diaphragma sella may allow further extension of the subarachnoid space through the foramina of the cribriform plate or around the hypophysis (empty sella). The former is common and accounts for the majority of normal pressure leaks.
Cerebrospinal leaks needs to be treated because of the impending threat of meningeal infections.
Figure showing AP view of ventricles
Figure showing various routes of CSF rhinorrhoea
Spontaneous CSF rhinorrhoea:
True spontaneous leaks are really rare. There is almost always some antecedent traumatic event.
Nuss postulated the various causes of spontaneous CSF rhinorrhoea. He named them as "4 P's".
1. Increased intracranial pressure
2. Brain pulsations which continuously occur along the skull base
3. Degree of pneumatisation of the paranasal sinuses
4. Arachnoid pits / villi exist normally along the skull base. Continued transmission of pulsation, erodes the bone until the arachnoid communicates with a pneumatised space with the potential to develop fistula.
Trauma: is the commonest etiology
Iatrogenic: Surgery involving skull base and paranasal sinuses may cause CSF rhinorrhoea due to breach in the skull base.
Congenital: Meningocele and Meningoencephalocele
Neoplasia
Bedsite tests for detecting CSF rhinorrhoea:
Reservoir sign: This test is ideally performed immediatly on rising from the bed. The patient is asked to place the chin over their chest. The patient must stay in that position for one full minute. Clear fluid dripping from the nose is CSF.
Handkerchief test: Discharge from the nose is blown into a handkerchief and is allowed to dry. If the discharge is CSF the handherchief will not stiffen, if the discharge is secretions from the nose the handkerchief stiffens due to the presence of mucin in the nasal secretions.
The most sensitive laboratory test is to look for Beta 2 transferrin in the nasal secretions. In CSF Beta 2 transferrin is present, and it is absent in normal nasal secretions.
The most sensitivve test to detect CSF leak is intrathecal radionucleotide test.
Tests that help to localise the CSF leak:
1. Flow sensitive MRI is useful. The leak must be active at the time of the scan for visualising the site. The advantage of this test is that it is non invasive.
2. Intra thecal administration of non ionic contrast with high resolution CT scan. Intra thecal administration of low quantities of flurescein can also be used. If the leak is present it can be viewed in the nasal cavity with a 490 nm light generated by a special optical filter. Dye injection is done using Barbolage technique in which 1 - 2 drops of 5 % Fluoresate is diluted with the patients own CSF, and then injected partially, then CSF is withdrawn further diluting the dye and then reinjecting the dye.
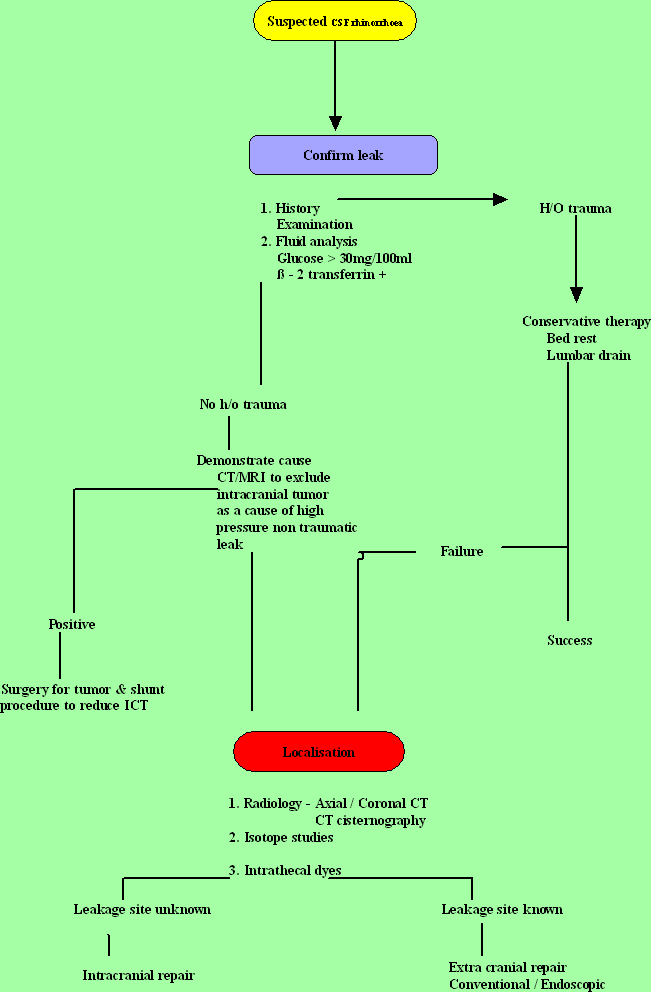
Management:
1. Bed rest
2. Elevation of the head end of the bed
3. Stool softeners
4. Short course of azetazolamide
5. Continuous / daily intermittent lumbar spinal drainage helps to reduce the fistula
6. Antibiotic prophylaxis to prevent meningitis.
Surgical management:
CSF leaks into the nose can be approached by two routes:
1. Intracranial repair
2. Extracranial repair
Intracranial repair: till recently this was the commonest approach adopted to repair CSF rhinorrhoea. Leaks from the anterior defects can be repaired by frontal anterior fossa craniotomy. A middle cranial fossa craniotomy or posterior fossa craniotomy can be used to mangage leaks from these areas. Leaks from the sphenoid sinus area are diffucult to approach via the intracranial route. The repair techniques involve use of a pedicled periosteal or dural flaps, muscle plugs can be used to plug the defects, mobilised portions of falx cerebri or other facial grafts can be utilised. Fibrin glue can be used to stabilise the grafts used in case of large leaks.
The advantages of this approach are
1. The adjacent brain tissue can be directly inspected
2. Direct visualisation of the dural defect
3. The repair can also be done even under conditions of increased intracranial tension
4. Even if efforts to localise the leak fails blind repair is possible in this approach. The areas covered with grafts must include the cribriform plate and the sphenoid sinus.
Disadvantages of this approach:
1. Increased morbidity
2. Increased risk of permanent anosmia
3. Trauma related to brain retraction (hematoma, oedema, seizures, cognitive dysfunction etc)
4. Longer hospital stay
Extracranial repair: This can be divided into external approaches and endoscopic techniques
External approach:
This include anterior osteoplastic approach via bicoronal or eyebrow incision, external ethmoidectomy, transethmoidal sphenoidectomy, and transeptal sphenoidectomy. Graft materials used could range from fascia lata, temproalis fascia, septal cartilage, turbinate mucosa, muscle and fat. For cribriform plate, or fovea leaks a transnasal ethmoidectomy is performed. For sphenoid leaks sphenoidectomy is performed.
Disadvantages of this procedure include:
1. Inability to repair associated intracranial abnormalities
2. Ineffective in repairing high pressure leaks
3. Ineffective in repairing frontal and sphenoid sinus leaks when they have prominent lateral extensions
Endoscopic techniques:
This method has several advantages including better visualisation and magnification. Other advantages include the ability to clean the mucosa adjacent to the leak, and in accurate positioning of the graft to plug the leak. There is no threat of anosmia, and this procedure has low morbidity.