Fungal Sinusitis
Definition: Fungi are eukaryotic organisms comprising of moulds, yeasts, mushrooms and other similar organisms. Among this group of organisms only about 0.1% are human pathogens. The term mycosis is used to define diseases caused by fungi.
Mycosis can be classified under 4 heads based on the portal of entry and site of infetion.
Types of mycosis:
Type |
Pathophysiology |
Route |
Example |
| Superficial | Limited to keratinized tissues | Topical | T. pedis |
| Subcutaneous | Localised to subcutaneous tissues | Broken skin | Rhinosporidiosis |
| Systemic | Disseminated widely | Inhalation | Histoplasmosis |
| Opportunistic | Local / Disseminated | Cell mediated immunity compromise | Candida / Mucormycosis |
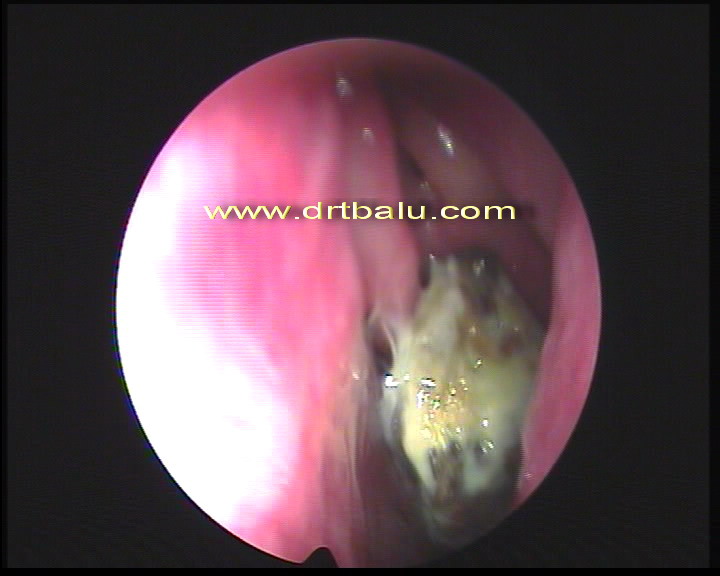
Endoscopic picture of Fungal Ball
Fungal infections of nose and sinuses are getting common these days. With increasing incidence of HIV and other diseases like diabetes which compromise host immunity it is no wonder that the incidence of fungal infections involving nose and para nasal sinuses is on the rise. In India the incidence of fungal sinusitis in immuno competent patients is also showing a rise. This particular fact need to be studied further.
Classification of fungal sinusitis: There are 5 different types of fungal sinusitis with differing pathophysiology and clinical presentation. They include:
1. Acute fulminant invasive sinusitis
2. Chronic invasive fungal sinusitis
3. Granulomatous invasive fungal sinusitis
4. Fungal ball
5. Allergic fungal rhino sinusitis
Recently one more group is added i.e. Eosinophilic fungal rhinosinusitis.
Acute fulminant invasive sinusitis: The whole duration of illness in these patients is just less than 4 weeks. These patients are mostly immunocompromised individuals. The reduced immunity could very well be a result of
a. Diabetes mellitus
b. AIDS
c. Immunosuppressive medicines
d. Malignancy causing immune suppression
The fungus commonly associated with this infection belongs to Mucoraceae family or Aspergillus family. If Mucor is involved then the lesion is angioinvasive and destroys both bone and soft tissue. Patients belonging to this group have high mortality rate. Extensive surgical debridement of the lesion with removal of necrotic tissue should be performed and must be followed with intravenous antifungal medication i.e. amphotericin B. If possible the underlying cause for immune compromise should also be addressed. Since granulocytes are essential to combat this condition, granulocyte infusions have been tried out with success after surgical debridement.
Chronic invasive fungal sinusitis: This condition is also known as Non granulomatous chronic invasive fungal sinusitis. This condition commonly afflicts patients with diabetis mellitus. This disorder is characterised by low grade inflammation with tissue necrosis. There is very little vascular invasion. Granuloma formation which is common in these patients requires an appropriate cell mediated immune response which is common in diabetics.
The duration of this disease is longer than 4 weeks (more than 6 weeks in some cases). Orbital extension is common, causing proptosis. These patients can be managed by wide surgical debridement, followed by systemic intravenous antifungal drugs like amphotericin B.
Granulomatous invasive fungal sinusitis: This condition is also known as Indolent fungal sinusitis. These patients have an intact cell mediated immune reponse. Clincially it is virtually impossible to distinguish it from non granulomatous fungal sinusitis. Histopathology will clinch the diagnosis. The intact immune system of the patient limits the invasion to the superficial mucosa. Granulomas could be seen surrounding the fungal elements thus preventing their deeper invasion. The granulomas could be seen surrounded by multinulceated giant cells, eosinophils etc. Surgical debridement alone is sufficient to cure these patients. Their intact immune system takes over from now on.
Fungal Ball: These mycetomas commonly present as unilateral opacification of maxillary or sphenoid sinus. The ethmoids and frontal sinuses are very rarely involved. These patients are usually immunocompetent without evidence of atopy. The fungal ball is composed of tightly packed hyphae often from Aspergillus, Alternaria and P. boydii. Treatment is mostly surgical removal of the fungal mass combined with widenening of ostium there by increasing the ventilation of the sinuses. Antifungal drugs are not indicated in these patients.
Allergic fungal sinusitis: These patients have a combination of nasal polyposis, crust formation associated with positive sinus cultures for aspergillus. Robson (1989) introduced the term allergic fungal sinusitis to describe the findings associated with this disease. These patients consistently demonstrate allergic reactions to aspergillus proteins.
Bent's criteria for the diagnosis of allergic fungal sinusitis:
1. Demonstrable type I hypersensitivity to fungi
2. Nasal polyposis
3. Radiological findings (Heterodense mass lesion)
4. Presence of eosinophilic mucin mixed with non invasive fungus
5. Positive fungal stain / fungal culture
These patients present with progressive nasal obstruction, crusting, rhinorrhoea, and chronic rhinosinusitis. These patients can also come with dramatic symptoms like visual loss and total nasal obstruction.
Classically radiology shows unilateraly expansile lesion of the sinuses associated with bony erosion. The mass appears as heterodense due to the presence of metallic elements in the fungal hyphae.
The mechanism of causation of allergic fungal sinusitis is IgE mediated hypersensitivity to fungal proteins especially to aspergillus.
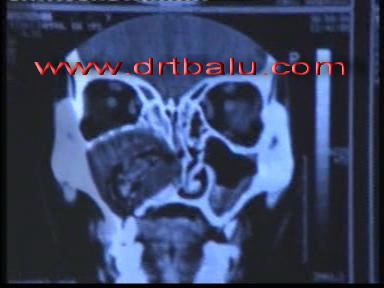
Coronal CT scan showing fungal sinusitis of right maxillary sinus
Note: Expansile lesion involving the right maxillary sinus. Erosion of medial wall of maxilla, the nasal cavity is filled with heterodense mass. The septum is seen being pushed to the opposite side.
Eosinophilic fungal sinusitis: This terminology was first suggested by Ponikau et al to explain the pathogenesis of not only allergic fungal sinusitis but also of chronic rhinosinusitis. This disorder is usually bilateral. Using sensitive techniques he was able to demonstrate the presence of fungal hyphae in 97% of cases with chronic rhinosinusitis. Since he failed to demonstrate typical type I allergic features like elevated IgE levels in sera he classified these patients under this head since he was not able to include them in the allergic fungal sinusitis group. He hence suggested an alternative theory saying that chronic sinusitis belonging to this group is caused by abnormal cell mediated response to fungal proteins.
Pathophysiology of eosinophilic fungal sinusitis:
In response to exposure to fungal proteins allergic mucin is formed in the mucosa. This allergic mucin attracts eosinophils from blood vessels. These eosinophils surround fungal hyphae and secrete substances like Major basic proteins and various interleukins.
Management of eosinophilic fungal sinusitis include surgical removal of polypi with creation of good antrostomy to improve ventilation of the sinuses. Oral steroids are indicated in these patients to prevent recurrence. Prednisolone is administered in doses of 0.1mg/kg/day in cylces of four days and is gradually tapered after 6 weeks. After tapering of oral steroids, topical nasal steriods can be administered for a period of 6 - 9 months.
Endoscopic staging of allergic fungal sinusitis
| Stage | Endoscopic picture |
| 0 | No mucosal odema or allergic mucin |
| 1 | Mucosal oedema with or without allergic mucin |
| 2 | Polypoid oedema with or without allergic mucin |
| 3 | Sinus polyposis with fungal debris and allergic mucin |
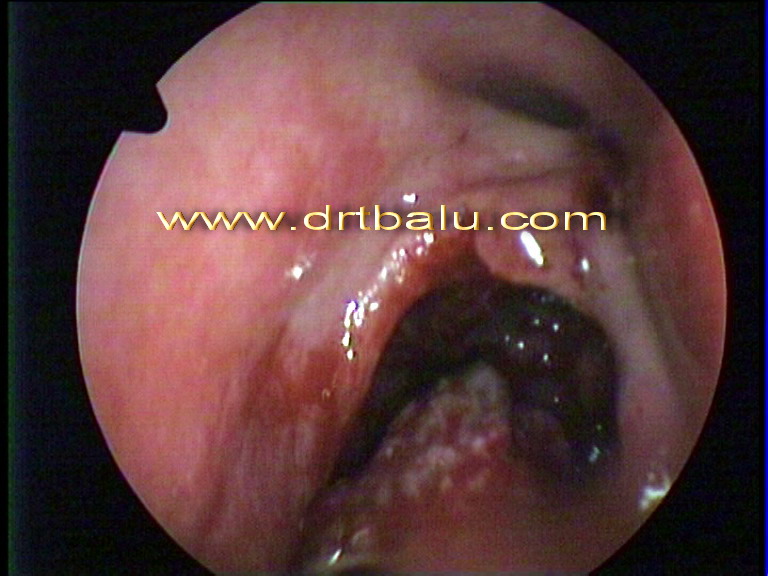
Endoscopic image of fungal sinusitis
