Glomus Jugulare
Synonyms: Paraganglioma, Chemodectoma, Ganglia tympanica, Vascular tumors of middle ear.
Definition: Glomus jugulare is defined as a collection of ganglionic tissue within the temporal bone in close relationship with the jugular bulb. The jugular bulb is closely related to the floor of the middle ear cavity (i.e. Hypotympanum).
History: Valentine in 1840 described this condition as ganglia tympanica. Guild recognised its histological relationship with the carotid body. Lattes and Waltner suggested that the ideal generic term for these structures is non-chromaffin paraganglioma.
Paraganglia cells are derived from the neural crest and are found widely distributed in the autonomic nervous system. Paraganglia having negative chromaffin reaction are termed non - chromaffin paraganglia. Guild in his anatomical studies on temporal bones found that on an average three glomus bodies were found in them. They were usually found in close relationship with the tympanic branch of glossopharyngeal nerve or the auricular branch of vagus. These bodies were supplied with non medullated sensory fibers from the adjacent nerves. They are supplied by branches from the ascending pharyngeal artery.
Eventhough the paraganglia cells are closely related to either the tympanic branch of glossopharyngeal nerve or the auricular branch of vagus, their position in the temporal bone is highly variable. Commonly they are found in the adventitial layer of the jugular bulb. In about 25% of cases they may be found over the mucosa of the promontory. Histologically, they resemble carotid body. It contains epitheloid cells interspaced in a highly vascular stroma of capillary and precapillary vessels. The proportion of the cellular and stromal components vary. Guild classified glomus tumors into two types depending on the amount of cellular and stromal components:
1. Cellular glomus bodies - when the cellular component is predominant
2. Vascular glomus bodies - when the vascular stromal component predominates.
Their sizes could be variable, but mostly they are ovoid in shape.
Paragangliomas of the temporal bone are generally divided into those that originate within the middle ear, glomus tympanicum tumors, and those that originate within the jugular fossa, glomus jugulare tumors. This latter term, however, is often used to refer to large tumors where the origin is difficult to determine. The predominance of the paraganglia within the jugular fossa likely accounts for the increased frequency of tumors with this origin. Classification systems that have been developed for temporal bone paragangliomas are used for staging purposes. surgical planning, and comparison among different therapeutic modalities.
Incidence: Glomus jugulare occurs in about 1 in 100000 patients. It is 6 times more common in females when compared to males.
Hereditary pattern: It shows autosomal dominant inheritance with variable penetrance.
Endocrine activity: Eventhough these tumors are considered non chromaffin paragangliomas with no endocrine activity, some cases with endocrine activity by these tumors have been reported. It is hence important to look for evidence of endocrine activity by urine estimation of VMA (Vanillylmandelic acid).
Glomus tumors sometimes may show multicentric presentation i.e. present in both ears, or in conjunction with other paragangliomas. The carotid body being commonly the second site.
Pathophysiology: Glomus tumors are encapsulated, highly vascular, and locally invasive tumors. Inside the temporal bone they tend to expand along the pathway of least resistance such as air cells, vascular lumen, skull base foramina and eustachean tube. They also invade and erode bone in a lobular fashion. The middle ear ossicles are commonly spared. Initially skull base erosion occur in the region of jugular fossa and postero inferior part of petrous bone. Later on extension occurs to the mastoid and adjacent occipital bone.
The parenchyma of the paraganglia consists of 2 primary cell types. Type I cells are more common and are typically round with indistinct cell borders. Type II cells are smaller and irregularly shaped.
Presentation: These tumors are slow growing, with very little symptoms. The diagnosis may easily be missed. Infact the average delay between the onset of symptoms and diagnosis varied from 6 years to 15 years. The first symptoms generally follow middle ear involvement is easily overlooked. Pulsatile tinnitus and conductive deafness are the common presenting symptoms. A red mass behind an intact ear drum (rising sun sign) may also be seen. In some 30% of cases cranial nerve palsies are common. Facial nerve is affected most commonly.
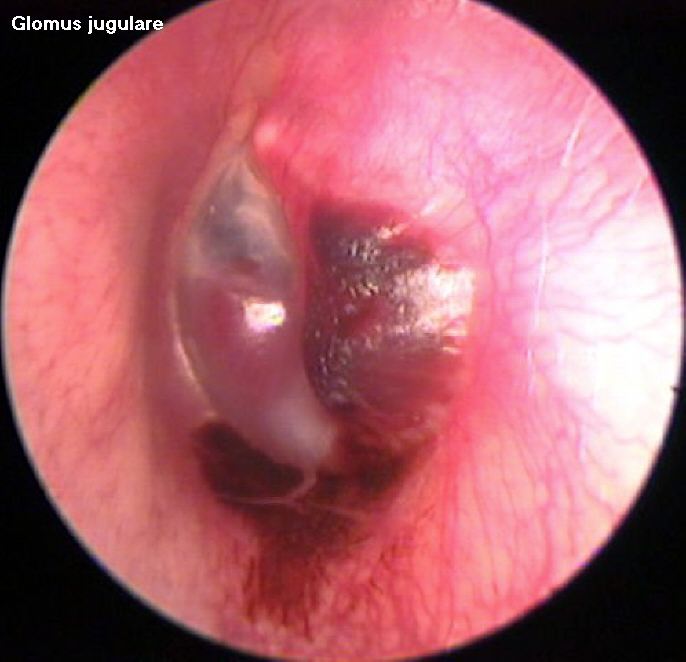
Otoendoscopic picture of Glomus jugulare
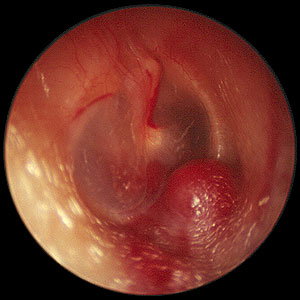
Glomus jugular with Rising sun sign
Presenting features of Gomus jugulare:
1. Deafness - 69%
2. Middle ear mass - 75%
3. Pulsatile tinnitus - 55%
4. Imbalance - 8%
5. Otorrhoea - 5%
6. Facial palsy - 8%
7. Endocrine syndrome - 3%
8. Cranial nerve deficits
Hoarseness - 16%
Dysphagia - 16%
9. Headache - 15%
10. Visual disturbance - 6%
11. Presence of headache indicates intracranial extension
12. Dural sinuses may be involved may mimic sinus thrombosis
Clinical features: Otoscopic examination reveals a characteristic, pulsatile, reddish-blue tumor behind the tympanic membrane that often is the beginning of more extensive findings (ie, the tip of the iceberg). When the drum is examined under a microscope will show a pulsation of the reddish mass behind the drum. On seigalisation the mass blanches. This sign is known as Brown's sign. This is pathognomonic of glomus tumor.
Audiologic examination reveals mixed conductive and sensorineural hearing loss. The sensorineural component tends to be more significant with larger tumors.
Classification:
Glasscock - Jackson classification of temporal bone paraganglioma:
1. Type I : Small tumor involving the jugular bulb, middle ear and mastoid.
2. Type II: Tumor extending under the internal auditory canal. There may be intracranial extension.
3. Type III: Tumor extending into the petrous apex. There may be intracranial extension.
4. Type IV: Tumor extending beyond the petrous apex into the clivus and infratemporal fossa. There may be intracranial extension.
The Fisch classification of glomus tumors is based on extension of the tumor to surrounding anatomic structures and is closely related to mortality and morbidity.
Fisch classification:
1. Type A tumor - Tumor limited to middle ear (carries the best prognosis)
2. Type B tumor - Tumor limited to the tympanomastoid area with no infralabyrinthine compartment involvement
3. Type C tumor - Tumor involving the infralabyrinthine compartment of temporal bone with extension to petrous apex
This is divided into three types: C1, C2 and C3.
Type C1 - Tumor with limited involvement of the vertical portion of the carotid canal
Type C2 - Tumor invading the vertical portion of the carotid canal
Type C3 - Tumor invasion of the horizontal portion of the carotid canal
4. Type D tumor has 2 types
Type D1 - Tumor with an intracranial extension less than 2 cm in diameter
Type D2 - Tumor with an intracranial extension greater than 2 cm in diameter
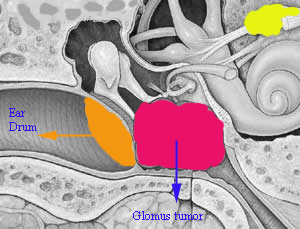
Image showing diagrammatic representation of Glomus
Investigations: Radiological investigations help in the diagnosis.
Plain X ray skull: May show enlargement of lateral jugular foramen and jugular fossa.
CT scan and Contrast MRI using Gadolinum enhancement is very helpful in delineating tumor extension.
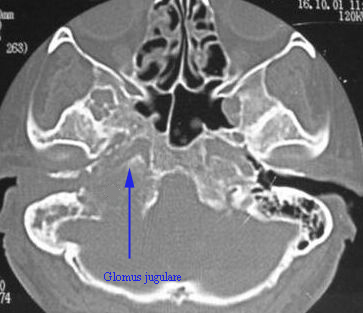
CT scan image of a patient with Glomus jugulare
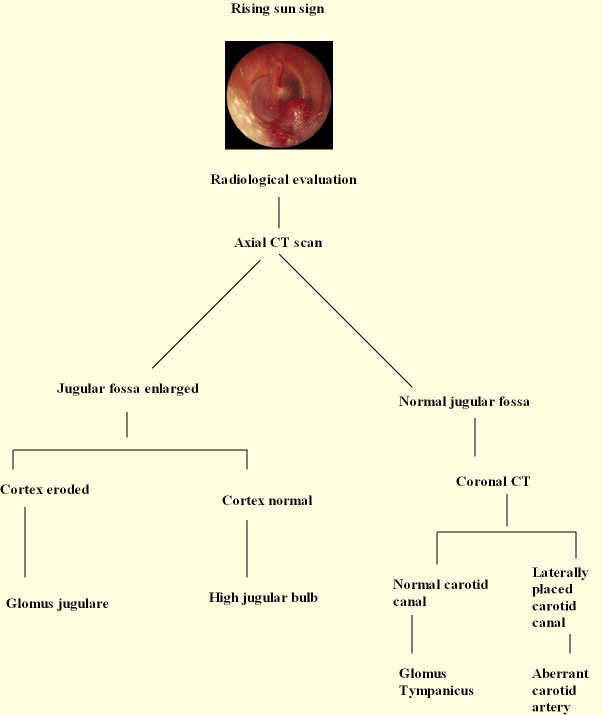
Flow chart showing radiological investigations to study glomus tumors in the middle ear
Applied anatomy of jugular bulb area:
The posterolateral portion of the foramen (pars venosa) contains the jugular bulb, posterior meningeal artery, and cranial nerves X and XI. The anteromedial portion (pars nervosa) contains the inferior petrosal sinus and cranial nerve IX. The jugular bulb is situated between the sigmoid sinus and the internal jugular vein. The lower cranial nerves are situated medial to the medial wall of the jugular bulb. The inferior petrosal sinus enters the medial aspect of the jugular bulb via several channels anterior to cranial nerves IX, X, and XI.
Many important structures are in proximity to the jugular bulb, including the internal auditory canal, the posterior semicircular canal, the middle ear, the medial external auditory canal, the facial nerve (posterolaterally), and the ICA (anteriorly) within the carotid canal. At the extracranial end of the jugular foramen, the ICA, internal jugular vein, and cranial nerves VII, X, XI, and XII are within a 2-cm area.
Treatment:
Treatment is mainly surgical. Complete resection of the mass is curative. Since it is a highly vascular tumor pre op intravascular embolisation may help to reduce bleeding during surgery.
The particular surgical approach used to resect temporal bone paragangliomas depends on the location and extent of the tumor. Paragangliomas originating from the promontory of the middle ear and isolated to the mesotympanum can be resected by elevating the tympanic membrane and removing the tumor using microdissection techniques. If the tumor extends into the hypotympanum or the mastoid, a tympanomastoidectomy is performed and the tumor resected.
In extensive Fisch type 3 tumors the mass can be approached with help from neurosurgeons. The skull base approach ensures better exposure of the mass and facilitates complete resection.
Management of Fisch type 4 tumors is highly controversial. Irradiation of the mass has been tried with very little effect. Considering the slow growth rate of these tumors with a very long doubling time, these patients are best left alone with symptomatic treatment of the complications.
Complications of surgery:
Complications of surgery include death, cranial nerve palsies, bleeding, cerebrospinal fluid (CSF) leak, meningitis, uncontrollable hypotension/hypertension, and tumor regrowth.
