Infratemporal Fossa
Synonyms: Ptreygopalatine fossa, infratemporal fossa
Definition: Infratemproal fossa is a potential space lying behind the maxilla.
Boundaries of infratemporal fossa:
Lateral: Bounded by Zygoma, the ramus of mandible, parotid gland and masseter muscle
Medial: Bounded by superior constrictor muscle, Pharyngobasilar fascia, Pterygoid plates
Anterior: The body of the maxilla lies anteriorly
Superior: Greater wing of sphenoid
Posterior: Auricular tubercle of the temporal bone, glenoid fossa and styloid process
The floor of the infratemporal fossa is closed by the medial pterygoid muscle.
The infratemporal fossa communicates superiorly with middle cranial fossa by the neurovascular formaina like carotid canal, jugular foramen, foramen spinosum, foramen ovale and foramen lacerum. Medially the infratemporal fossa communicates with pterygopalatine fossa through the pterygomaxillary fissure. The pterygomaxillary fissure is contiguous with that of the infraorbital fissure. The roof of the infratemporal fossa is open to the temporal fossa lateral to the greater wing of sphenoid, deep to the zygomatic arch.
Benign tumors involving the infratemporal fossa always respect these boundaries and expand in the direction of soft tissue planes, or follow preexistant pathways and foramen described above.
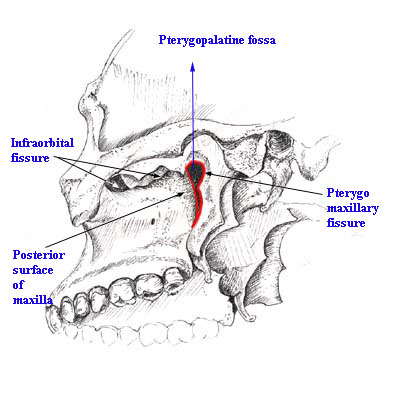
Image showing pterygopalatine fossa
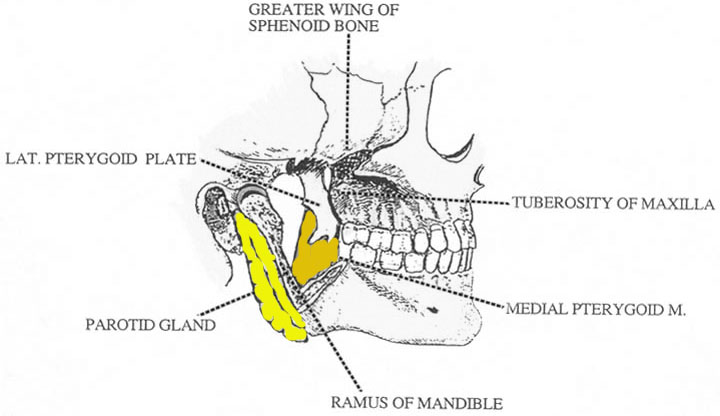
Figure showing boundaries of infratemporal fossa
Contents of infratemporal fossa:
1. Lateral pterygoid muscle. This is the largest component of the infratemporal fossa. This muscle has two heads, upper and lower. The upper head is smaller and arises from the greater wing of sphenoid, while the larger lower head arises from the lateral aspect of lateral pterygoid plate. The fibers of both these heads pass backwards to be inserted into the neck of the mandible. The action of lateral pterygoid muscle i.e. protrusion of the lower jaw can easily be tested during clinical examination of the patient.
2. Temporalis muscle: This muscle occupies a wedge shaped space just lateral to the lateral pterygoid muscle.
3. Pterygoid venous plexus: There is rich plexus of veins seen in this space. It lies admixed with fatty tissue seen in the infratemporal fossa. These plexus could cause troublesome bleeding during total maxillectomy surgery.
4. Infratemporal pad of fat: Lies between the temporalis muscle and the infratemporal surface of maxilla. The pad of fat helps in outlining the posterior antral tumor spread in CT scans. This infratemporal pad of fat continues with the cheek pad of fat passing between the posterior wall of maxilla and the zygoma. A mass present behind the maxilla always betrays itself by displacing this pad of fat and causing a puffy swelling of cheek (i.e. angiofibroma).
Axial CT image showing JNA mass
5. Buccal lymph node: Within this infratemporal pad of fat lies the buccal lymph node. This node links the infratemporal lymphatics to the facial lymphatics. This node should never be left behind during surgical resection of infratemporal fossa for malignant tumors as it could commonly cause local recurrence.
6. Mandibular nerve penetrates the roof of the infratemporal fossa through the foramen ovale. It also gives rise to inferior alveolar and lingual nerve branches.
7. Internal maxillary artery and its branches lies on the superficial or deep surface of the lateral pterygoid muscle.
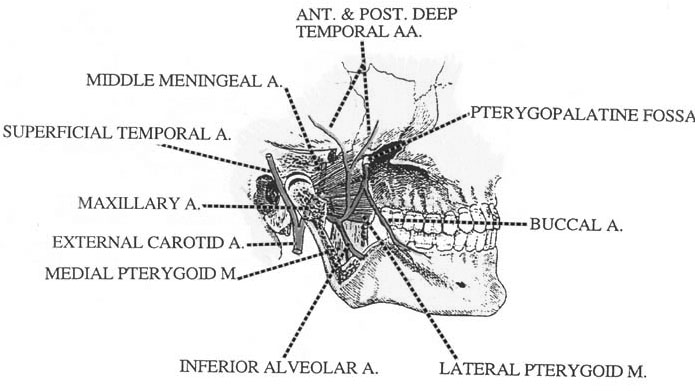
Image showing internal maxillary artery and its branches
Tumors involving infratemporal fossa present with a variety of symptoms depending on the structure involved. It could be a mass effect, eustachean tube dysfunction, cranial neuropathies, trismus etc. The corner stone of diagnosis of tumors of this area is imaging which includes a CT scan and MRI.
Surgical approach to infratemporal fossa: It was Barbosa in 1961 who described an approach to expose this space. He extended the orbital limb of the radical maxillectomy incision horizontally backwards up to the pretragal region. After raising the parotid off the masseter, the maxillary artery was ligated. The temporalis muscle was sectioned at the upper margin of the zygomatic arch and the masseter was divided below the arch. The zygomatic arch was freed. The ramus of the mandible along with the head was detached by a horizontal mandibular osteotomy at the level of the teeth. The space is entered by mobilising the block of mandible and its attached muscle forwards.
Pterygopalatine fossa:
This space lies between the posterior wall of the maxilla and the anterior face of the pterygoid process. This is a small but very important distribution center for the nasal cavity and the middle 1/3 of the face. Sensory, secretomotor, and vasoregulatory nerves pass through this niche on their way from the middle cranial fossa to the face, teeth, palate, turbinates, sinuses, lacrimal glands and nasopharynx. Entrance to the pterygopalatine fossa from the infratemporal fossa is through the pterygomaxillary fissure.
Cancers in the pterygopalatine fossa has ready access to the middle cranial fossa via the foramen rotundum. The lesion here could also reach the orbital apex through the infraorbital fissure, which is nothing but the open roof of the pterygopalatine fossa. Lateral spread of tumors from this space could involve the infratemporal fossa. Nasopharynx could be involved by medial infiltration of the tumor via the sphenopalatine foramen. Hence involvement of the pterygopalatine fossa is really ominous in patients with paranasal sinus neoplasia.
A small parasympathetic ganglion (sphenopalatine ganglion) lies suspended in this space from the maxillary nerve. The following features are commonly seen when the pterygopalatine fossa is invaded by a malignant mass:
1. Deep facial pain
2. Hard palate insensitivity
3. Decreased lacrimation
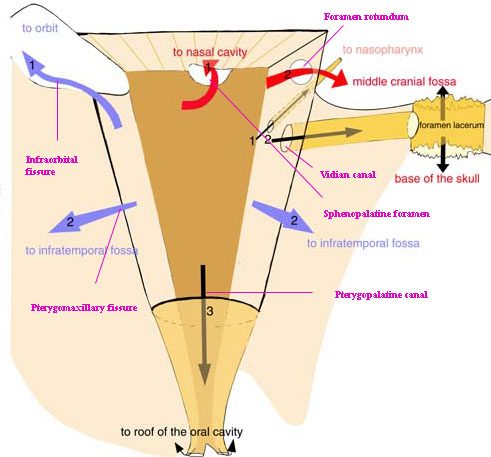
Image showing openings of pterygopalatine fossa
