Inverted Papilloma
Synonyms: Schneiderian papilloma, Benign papilloma of nasal cavity, Inverted papilloma.
Definition: The mucosal lining of nose and para nasal sinuses is known as Schneiderian membrane, in memory of Victor Conrod Schnider who described its histology. Papillomas arising from this membrane is very unique in that they are found to be growing inwardly and hence the term inverted papilloma. These papillomas are unique in their history, biology and location.
Papillomas involving the vestibule is not included under this group because histologically, biologically and behaviour wise it is different.
The lining mucosa of nose and paranasal sinuses is unique embryologically in the sense that it is derived from the ectoderm, in contrast to the lining epithelium of laryngobronchial tree which is derived from endoderm.
Inverted papillomas behave like neoplasms, arising from reserve / replacement cells located at the basement membrane of the mucosa. The stimulus for this proliferation is unknown. The resulting thickening of the epithelium assumes an inverting, fungiform or combination growth pattern. Depending on the degree of metaplasia varying amounts of respiratory / cylinderical cells may be seen in schneiderian papilloma. Rarely the papilloma may be composed entirely of cylinderical cells, and hence the term cylinderical cell papilloma is used to describe this subtype.
Anatomic classification of Schneiderian papilloma: Inverted papilloma can be classified according to its site of occurance i.e. lateral wall and septal papillomas. They show differences in their behavior patterns. The septal papillomas remain confined to the nasal septum and may very rarely involve the roof and floor of the nasal cavity. Carcinomatous transformation is rare in septal papillomas.
Papilloma of lateral wall is known to involve multiple sites i.e. floor, roof of nasal cavity, para nasal sinuses and naso lacrimal duct. Carcinomatous transformation is common in this variety.
Clinical classification of inverted papilloma was proposed by Krouse. He used his classification and staging protocol to decide on the optimal treatment modality of these patients.
Krouse classification:
T1 - The disease is limited to the nasal cavity alone
T2 - Disease is limited to ethmoid sinuses and medial and superior portions of maxillary sinuses
T3 - Disease involves the lateral or inferior aspects of maxillary sinus or extension into frontal or sphenoid sinuses
T4 - This stage involves tumor spread outside the confines of nose and sinuses. This stage also includes malignancy
Incidence: Inverted papillomas are fairly common occurring in 1 - 50 of patients with nasal polypi. If all nasal polypi removed surgically are tested histopathologically then the incidence could be still more higher. Men are affected more commonly than women. The age of affliction may range from between second to seventh decade of life. The mean age of presentation being 50.
Etiology: Human papilloma virus has been implicated as a causative factor in these patients. This infection in association with mutation of genes may cause papillomas. Coinfection with Herpes simplex virus may interact with Human papilloma virus to cause inverted papilloma.
Role of imaging in the diagnosis of inverted papilloma:
CT scan is necessary for determining the optimal surgical approach in managing these patients. It also has the added advantage of differentiating other mass lesions involving the nasal cavities. Classically inverted papillomas occupies the middle meatus and lateral nasal wall with areas of higher density associated with bony sclerosis. If contrast is used for CT imaging contrast enhancement is also seen.
MRI: Is very useful when the tumor has extrasinosal involvment or show malignant transformation. It also helps in the differentiation of tumor tissue from inflammatory mucosa.
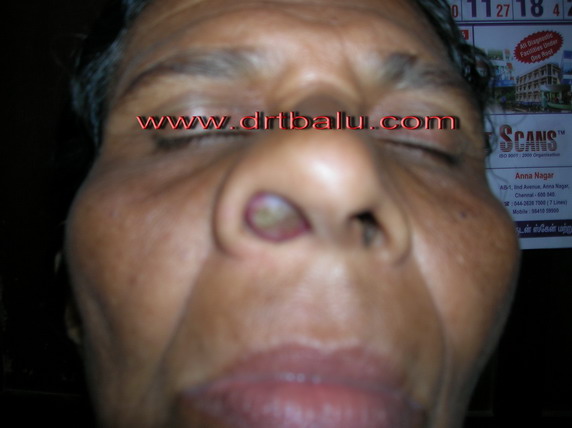
Image showing inverted papilloma right nasal cavity

Gross appearance of inverted papilloma
Gross apprearance: Nasal papillomas show two architectural patterns: 1. Papillary and exophytic 2. Inverted with inwardly invaginating epithelial growth into underlying stroma. A combination of both patterns also can occur. The papillary form tends to commonly occur in the nasal septum, while the inverted form often occurs in the lateral wall of the nose and sinuses.
Microscopy: The papillary form also known as fungiform papilloma shows epithelial proliferation over a thin core of connective tissue. Inversion of epithelial masses is usually not present. In the case of inverted papilloma the predominant growth is directed inwards into the underlying stroma. The stroma is not breached in these patients. When they undergo malignant transformation the stroma is found to be breached. The predominant cell type in these papillomas is epidermoid in nature. Intercellular bridges can be clearly demonstrated. Microscopic mucous cysts can also be identified in both these types. Keratinisation is very minimal. Excessive keratinisation is very rare, and should prompt the pathologist to other diagnosis like malignant transformation.
Clinical features: Patients present with unilateral nasal mass, commonly fleshy in nature. Sometimes it may occur behind a sentinel nasal polyp. It commonly involves the nasal cavity, erodes the medial wall of maxilla and may present inside the maxillay sinus.
Symptoms: are usually caused by compression of adjacent structures like orbit, pterygopalatine fossa, base of skull or soft tissues.
1. Unilateral nasal obstruction
2. Nasal bleeding
3. Nasal discharge
4. Proptosis if lamina papyracea is breached
Management: Surgical removal provides cure in most of the cases. Recurrence is common in 20% of patients. It is commonly removed pervia naturalis. If the mass is huge then lateral rhinotomy will have to be resorted to for complete removal.
Complications:
1. Haemorrhage
2. Malignant transformation
