Nasal Resistance
Introduction: Airway resistance is a very important factor which prevents total collapse of the lung. A totally collapsed lung causes intense difficulties during respiration. In adults 2/3 of the total airway resistance is provided by the nose. Infact this can even be considered as one of the functions of the nose in addition to olfaction, and airconditioning.
The components of nasal resistance are:
1. Nasal vestibule
2. Nasal valve area
3. Turbianted nasal passages
Nasal vestibule - has compliant walls, hence it has a tendency to collapse in response to the negative pressure caused during inspiration. This collapse of the compliant walls limits the nasal airflow in this segment. This area can hence be considered as a flow limiting segment of the nose (starling resistor). This resistance occur only during inspiration as expiratory flow causes positive pressure within the vestibule.
Nasal valve - This area is the narrowest portion of the whole of the nasal cavity and offers the maximum resistance to the nasal airway. This area is referred to as the nasal valve area. Anatomically this area lies just anterior to the inferior turbinate. The dimensions of the nasal valve area is maintained by the inferior turbinate and the corresponding portion of the nasal septum. The inferior turbinate is made up of venous erectile tissue, which determines the size of the turbinate. Any treatment aimed at reducing the swelling of the inferior turbiante will have major effects on nasal resistance, whereas any corrective surgery like trimming of septal spurs posterior to the nasal valve region will have very little effect on nasal resistance.
Turbinated nasal passages: The turbinates of the nose can change their shape thereby reducing the dimensions of the nasal cavity contributing to nasal airway resistance.
How is the nasal resistance controlled?
In normal healthy subjects the nasal airway resistance is determined by the degree of engorgement of venous erectile tissue, as well as the accessory muscles of respiration which keep the nasal airway patent. The venous erectile tissue of nasal mucosa has dense adrenergic innervation which when stimulated cause intense vasoconstriction thereby decreasing the nasal airway resistance. Normally there is a continuous sympathetic vasoconstrictor tone to the nasal erectile tissue keeping the nasal airway resistance under check. Reduction in this sympathetic tone increases the nasal airway resistance. The parasympathetic tone in the nose controls nasal secretion, but has little role in nasal resistance.
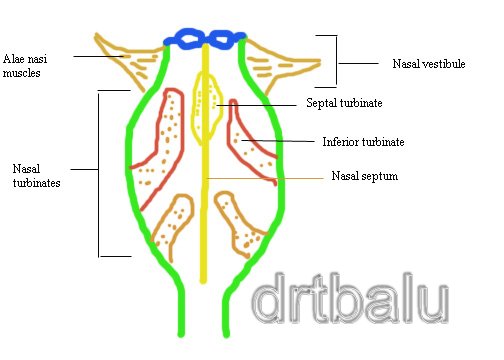
Image showing contributors of nasal resistance
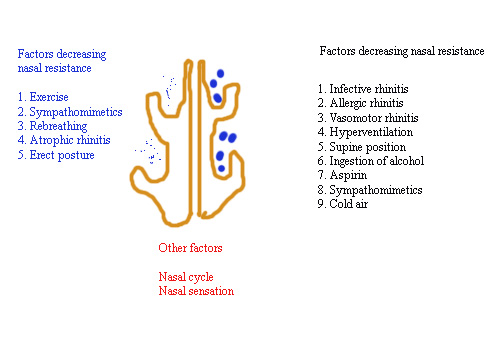
Image showing factors determining nasal resistance
Nasal air flow receptors are present in the nasal vestibule, these receptors are supplied by infra orbital branch of trigeminal nerve. The sensation of nasal air flow is greatly enhanced by stimulation of these receptors. Menthol is one such stimulant. When balm containing menthol is applied outside the nasal cavity it stimulates these receptors increasing their sensation to nasal airway causing symptomatic improvement.
Methods of measuring nasal airway resistance:
1. Rhinomanometry is used to assess the patency of the nose. There are two types of rhinomanometry, active and passive rhinomanometry. Active rhinomanometry involves the generation of nasal airflow and pressure with normal breathing. Passive rhinomanometry involves the generation of nasal airflow and pressure from an external source, such as fan or pump which drives air through the nose.
Active rhinomanometry: can be divided into anterior and posterior methods according to the siting of the sensor tube. In active anterior rhinomanometry, the pressure sensing tube is taped to one nasal passage. This method measures resistance of one nasal cavity at a time and must be repeated on the other side. The total air flow through the nose is measured with the help of the sensor tube. In active posterior rhinomanometry, the pressure sensing tube is held within the mouth and it detects the post nasal pressure. Air flow through each nose can be measured by taping the opposite nose.
Precautions taken while performing rhinomanometry:
a. The use of face mask is desirable than a nasal cannula. The face mask should form a soft air tight seal and must not effect pull on the cheek.
b. Calibration of the equipment must be performed regularly.
c. Series of readings must be taken as a single reading is unreliable.
2. Acoustic rhinometry: is performed by generating an acoustic pulse from a speaker which is transmitted along a tube into the nose. The sound from the pulse wave is reflected back from inside the nose and is related to the cross sectional area of the nasal cavity. The reflected sound is recorded by a microphone and calculations are made accordingly. It gives a precise estimation of the nasal cross sectional area.
3. Nasometry: During speech sound is transmitted through both the oral and nasal cavities. Nasal obstruction causes a reduction in the amount of sound transmitted through the nose. By measuring the nasal components of speech the patency of the nasal airway can be assessed. This is known as nasalance. It is the ratio of sound energy from the nasal and oral passages and can be measured by placing two microphones one over the nose and the other over the mouth. Infact the measure of nasalance has been proposed as a useful method of selecting children for adenoidectomy. It is also useful in measuring the nasal airway patency.
