Otosclerosis
Synonyms: Otospongiosis, Ankylosis of foot plate of stapes.
Definition: Otosclerosis is a hereditary localised disease of the bone derived from the otic capsule characterised by alternating phases of bone resorption and new bone formation. The mature lamellar bone is removed by osteoclasis and replaced by woven bone of greater thickness, cellularity and vascularity.
History: In 1741 Antonio Valsalva described ankylosis of stapes while doing a postmortem on the body of a deaf patient.
In 1894, Adam Politzer introduced the term "otosclerosis" and described the histopathology of the disease for the first time.
In 1912 Siebenmann introduced the term otospongiosis to denote active otosclerotic foci.
Pathophysiology:
The primary pathological change occurs in the bony labyrinth with secondary effects upon middle ear and inner ear function. The otosclerotic focus may be asymptomatic, or if present in the area of foot plate of stapes it may give rise to ankylosis of foot plate with resultant conductive deafness. Otosclerotic foci may involve other portions of labyrinth causing sensori neural hearing loss and vestibular abnormalities.
A combination of effects are possible in otosclerosis. They are:
Histological otosclerosis: Otosclerotic foci doesnot cause any symptoms and hence known as histological otosclerosis.
Stapedial otosclerosis: is the classical otosclerosis with fixation of stapedial foot plate causing conductive deafness.
Cochlear otosclerosis: The foci involves the cochlea causing sensorineural deafness.
Combined otosclerosis: Here in addition to fixation of foot plate of stapes there is also associated sensorineural hearing loss due to involvement of cochlea.
Otospongiosis: European otologists prefer to use this term to indicate the active phase of otosclerosis.
Incidence: Otosclerosis is common in caucasian races. It is rarely found in Mongoloid and Negro population.
Sex incidence: In clinical practice otosclerosis is seen more often in women than in men. The ratio was found to be 2:1. Nowadays the authors believe the apparent female preponderance may be due to the fact that unilateral otosclerotic deafness is less common in women than in men. Noticeable deterioration in hearing also occur during pregnancy due to hormonal changes. Deafness due to otosclerosis may be initiated or made worse by pregnancy.Causative factors / etiology: Many theories have been proposed to explain the etiological factors of otosclerosis. They are:
1. Metabolic
2. Immune disorders
3. Vascular disease
4. Infection (Measles) currently accepted
5. Trauma : The petrous bone doesnot have regenerative capacity. This is because of the fact that the enzymes released during reparative phase are very toxic to the inner ear hair cells.
Pockets of tissue capable of regeneration may be sequestered in various portions of labyrinthine bone. These tissue could be activated by the presence of regenerative enzymes in the blood following bone fracture elsewhere in the body.
6. Temporal bone abnormalities (congenital)
Genetic factors predisposing to otosclerosis: The tendency for otosclerosis to run in families has been documented. Authors have postulated an autosomal dominant mode of inheritance with varying degrees of penetration.
Otosclerosis is associated with osteogenesis imperfecta in 0.15 % of cases. This is known as Van der Hoeve syndrome or Adair - Dighton syndrome.
Sites affected by otosclerosis: The commonest site for apperance of otosclerotic bone is fissula ante fenestrum. This fissula is constantly seen in the labyrinthine capsule lying in front of the oval window. This area may contain unossified cartilage persisting even in adults. This area was referred to as Cozzolino's zone by Perozzi in memory of his teacher. Otosclerosis may occur in this area due to bony ossification of the cartilage.
Residual cartilage may be present in the following areas of labyrinth:
1. Fissula ante fenestram
2. Fissula post fenestram
3. Intracochlear
4. Round window
5. Semicirular canals
6. Petrosquamous suture
7. Base of styloid process
In normal development the fissula appears as fibrous connective tissue bundle joining the vestibule with the tympanic cavity. This fibrous tissue is encased in primary cartilage which later gets replaced by bone. From the fissula the bone acquires a connective tissue lining which later becomes converted into perichondrium. The fissula is reduced in size by the production of new secondary cartilage from the perichondrium. These changes are completed by birth. The secondary cartilage remains throughout life as a stable, dormant cartilage and hence may even be considered as normal structure. It is only when this secondary cartilage gets ossified otosclerosis occur (Bast & Anson).
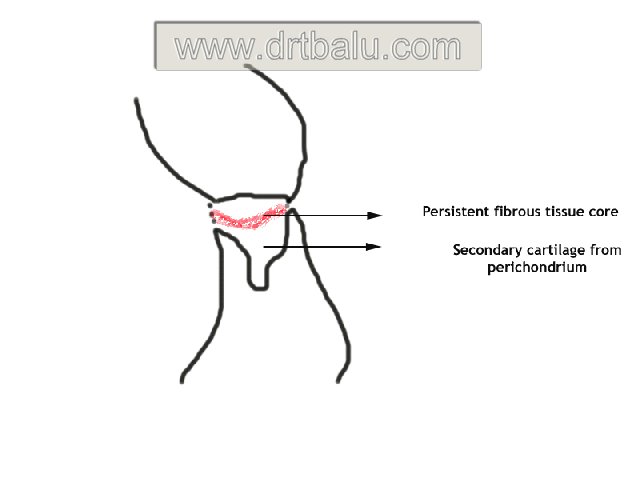
Diagramatic representation of fissula ante fenestram
Otosclerotic changes may appear as a result of interaction between bone growth promoting substances circulating in the blood stream, and the unstable cartilagenous elements in the capsule of the labyrinth. Otosclerosis is often seen at times when the bone growth promoting substances are circulating in the blood as in pregnancy and following fractures of other bones.
Histopathology of otosclerosis:
The normal endochondral bone of labyrinthine capsule in which otosclerotic focus begins is compact in type. Ultrastructurally, lamellae composed of fine fibrils lying in a ground substance are concentrically disposed around haversian canals containing blood vessels and connective tissue. In otosclerosis there is sharply defined new bone formations that could be differentiated from normal bone by their deep carmine stain and by marked enlargement of bone spaces and haversian canals. The following are the changes which occur in a otosclerotic foci:
1. Focal / diffuse replacement of normal compact bone by irregular, loose cancellous bone with more deeply staining lamellae.
2. There is an associated increase in size of Haversian canals, cell spaces and marrow spaces with corresponding increase in vascularity. The blood vessels are frequently surrounded by a narrow margin of blue staining material that Manassee described first as Blue Mantle zone.
3. Increase in osteocytes, and appearance of osteoblasts and osteoclast cells.
Histologically otosclerosis may be classified into:
1. Early focal otosclerosis
2. Diffuse active otosclerosis
3. Quiescent otosclerosis
4. Cochlear otosclerosis
Early focal otosclerosis: In this type the abnormalities are localised to one or two small areas of an otherwise normal foot plate section. The abnormal areas show an enlarged marrow space surrounded by a blue staining area on H&E staining.
Diffuse active otosclerosis: In this type there is abnormal vascularity with a great increase in size and number of marrow spaces. Most of these spaces are lined by osteoblasts. In places around the circumference of the marrow spaces there is a scalloped appearance where bone has been recently absorbed. The number of osteocytes are greatly increased.
Quiescent otosclerosis: Here eventhough there may be some increase in the size and number of marrow spaces there is no evidence of bone formation or bone destruction. Osteoblasts and osteoclasts are only occasionally seen. This could be considered as a burnt out phase of the disease spectrum.
Cochlear otosclerosis: This condition causes pure sensorineural deafness without stapes fixation. Otosclerotic foci may occur in the otic capsule without the involvement of stapedial foot plate. The process of bone erosion and new bone formation which occur in otosclerosis releases enzymes like amylase, SGOT, SGPT etc which can enter into the endolymph via the round window membrane. These enzymes are toxic to the sensitive hair cells of the cochlea causing sensorineural hearing loss.
Clinical types of otosclerosis: Classification of various clinical types of otosclerosis is based on microscopic appearances of the diseased foot plate.
Rim fixation: Here the otosclerotic foci starts from the anterior portion of the oval window niche. It gradually expands to involve the anterior portion of the foot plate causing fixation of the anterior portion of the foot plate only leaving the centre of the plate free.
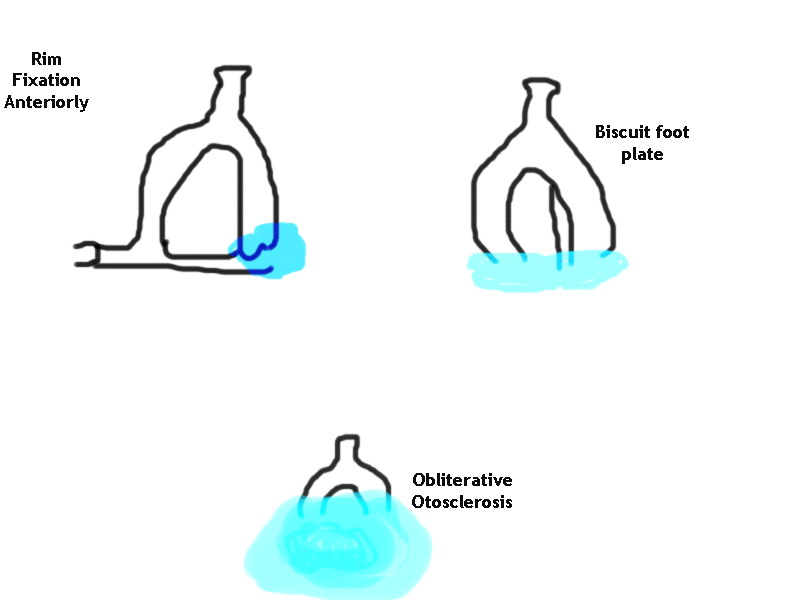
Diagramatic representation of various clinical types of otosclerosis
Biscuit foot plate: This type occur less frequently. The focus originates in the foot plate itself and as it expands it gives rise to the biscuit or rice grain foot plate with delineated margins.
Obliterative otosclerosis: Rarely a large mass of otosclerotic new bone fills up the oval window niche obscuring the entire foot plate. This condition is known as obliterative otosclerosis. It is a difficult condition to manage surgically.
Clinical features:
Deafness: Typically deafness in otosclerosis is bilateral and gradually increasing in nature. Unilateral otosclerosis occur in 15% of patients. Frequently it occurs between third and fifth decades of life. In majority of cases the deafness is conductive in nature. The deafness will not be noticed by the patient till the loss reaches 30 dB level. This is the deafness level in which understanding speech becomes difficult. These patients may hear better in noisy environment because the speaker has a tendency to raise his voice because of excessive ambient noise. This phenomenon a feature of otosclerosis is known as Paracusis Willisii.
In cochlear otosclerosis the deafness is purely sensorineural in nature. Some patients may have both conductive and sensorineural hearing loss (mixed deafness) because of the tendency of bone reparative enzymes to damage the inner hair cells.
Patients with otosclerosis have characteristically quiet voice with good tone and the change in speech pattern may be detected only by close relatives.
Tinnitus: is a common symptom and occasionally could be the only presenting feature. The presence of tinnitus should alert the physician about the presence of cochlear otosclerosis. It could also be seen in some patients without cochlear degeneration due to abnormally increased vascularity of the otosclerotic bone. Mostly tinnitus indicates sensorineural degeneration. Tinnitus may be unilateral or bilateral. It is usually roaring in nature.
Vertigo: Transient attacks of vertigo is not uncommon in patients with otoslerosis. This could be due to the action of toxic enzymes released by the lesion into the vestibular labyrinth. These patients may even have coexisting Meniere's disease.
Clinical examination: The ear drum in these patients is normal (mint condition). Rarely during active phase of the disease the increased vascularity of the promontory may be seen through the ear drum. This sign is known as Flemingo's flush sign or Schwartz's sign. This indicates otospongiosis (active otosclerosis).
Hearing assessment can be done using tuning forks. For detailed description of tuning fork tests read the chapter titled clinical examination of the ear.
Pure tone auditometry will show precisely the amount and type of hearing loss. The presence of Carhart's notch is a classic audiometric feature in these patients. This Carhart's notch is present in bone condution. There is a dip centered around 2000 Hz. This is actually an artifact. In cochlear otosclerosis audiometry reveals sensorineural hearing loss.
Stapes fixation causes an elevation in the bone conduction thresholds of 5dB at 500Hz, 10dB at 1000 Hz, 15 dB at 2000 Hz, and 5 dB at 4000 Hz. In the audiogram this creates a peculiar pattern known as Cookie bite audiogram. The bone conduction audiogram appears like a cookie having been bitten.
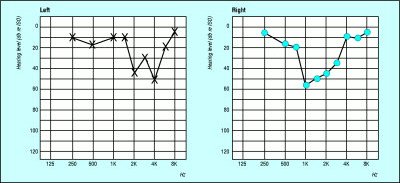
Figure showing Cookie bite audiogram a feature of otosclerosis
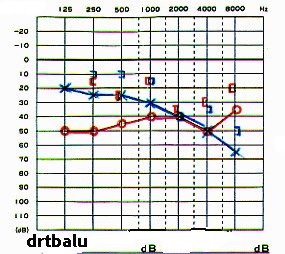
Audiogram showing carahart's notch a feature of otosclerosis
Impedence audiometry is an useful investigation to diagnose otosclerosis. Middle ear compliance is often reduced. When stapes is fixed stapedial reflex is absent. The typical impedence curve is As curve.
All these patients with pure conductive deafness have excellent speech discrimination thresholds.
Management:
Medical: The aim of medical management is to convert an active otosclerotic foci into an inactive or quiscent foci. Fluride is the drug of choice.
Indications of fluride therapy:
1. Patients with surgically confirmed otosclerosis who show progressive sensorineural deafness disproportionate to age.
2. Patients with pure sensorineural loss with family history, age of onset, audiometric pattern and good auditory discrimination indicate the possibility of cochlear otosclerosis.
3. Patients with radiological demonstration by CT scan of spongiotic changes in the cochlear capsule
4. Patients with positive Schwartz sign.
5. Post op treatment: If patients are found to have an active focus during surgery, fluride therapy is prescribed for 2 years.
Contraindications of fluride therapy:
1. Patients with chronic nephritis and nitrogen retention
2. Patients with chronic rheumatoid arthritis
3. Patient who are pregnant / lactating
4. In children before skeletal growth has been completed
5. Patients who show allergy for the drug
6. Patients with skeletal flurosis
Flurides act on otosclerotic foci by reducing osteoclastic bone resorption with a corresponding increase in osteoblastic bone formation. Fluride also has antienzymatic action thereby it can neutralise the toxic enzymes released from the otospongiotic foci.
Dose: A daily dose of 50 mg of sodium fluride is given for a period of 2 years. In patients with positive Schwartz's sign the dose can be increased up to 75 mg per day.
Adverse effects of sodium fluride therapy:
1. Gastric disturbance
2. Arthritis
3. Skeletal flurosis
Surgical treatment: Stapedectomy
Hearing aids: These patients will benefit from the use of hearing aids if surgery is not acceptable to the patient or if it is risky. There is always a 1% risk of producing a dead ear during surgery even in the best of hands.
