Malignant Tumors of Salivary Glands
Introduction: Malignant tumors involving the salivary glands are challenging to treat because of the following reasons:
1. Diversity of histological types
2. Anatomical constraints
3. Rarity of these tumors
Very few epidemiological studies are available which could throw light on the incidence of these tumors. Most commonly quoted data is from the swedish study (retrospective data from 1960 - 1989) puts the incidence to be about 0.3% of all diagnosed cancers. The incidence of malignancy is relatively higher in the submandibular, sublingual and minor salivary glands. Approximately 85% of sublingual gland tumors are malignant. Majority of tumors involving the parotid gland are benign.
Etiology of salivary gland cancers:
1. Increased alcohol consumption
2. Increased smoking
3. Smoking and alcoholism has a cumulative effect in causing salivary gland cancers
4. Exposure to aflotoxins. Salivary gland cancers are common in workers working in life stock feed processing units. This has been attributed to the presence of excessive amounts of aflotoxin B1 present in the feed. Infact aflotoxin happens to be a contaminent in the life stock feed.
5. Exposure to radiation
6. Ebstein Barr virus infections
7. Diet and nutritional habits: Intake of polyunsaturated fatty acids have a protective effect from these cancers
Theories of cellular origin of salivary gland malignancy:
Two theories predominate in the study of cellular orgin of salivary gland malignancy. They are:
Bicellular stem cell theory: This theory postulates that tumors arise form one of the two undifferentiated stem cells, the excretory duct reserve cell or the intercalated duct reserve cell. Excretory stem cells give rise to squamous cell and mucoepidermoid carcinomas, while intercalated stem cells give rise to pleomorphic adenomas, oncocytomas, adenoid cystic carcinomas, adenocarcinomas, and acinic cell carcinomas.
Multicellular theory: This theory assumes that each tumor type is associated with a specific differentiated cell of origin within the salivary gland unit. Squamous cell carcinomas arise from excretory duct cells, pleomorphic adenomas arise from the intercalated duct cells, oncocytomas arise from the striated duct cells, and acinic cell carcinomas arise from acinar cells.
Recent evidence suggests that the bicellular stem cell theory is the more probable etiology of salivary gland neoplasms. This theory more logically explains neoplasms that contain multiple discrete cell types, such as pleomorphic adenomas and Warthin tumors.
Role of oncogenes in the pathogenesis of salivary gland tumors:
1. Tumor suppresor genes belonging to p53 family play an important role in the development of salivary gland tumors. Mutations involving genes of this family has been known to cause salivary gland malignancy.
2. Murine double minute 2 (MDM2) a cellular protooncogene if amplified is capable of causing tumerogenesis by inactivating p53 tumor suppressor gene.
3. Hepatocyte growth factor (HGF), a protein that causes morphogenesis and dispersion of epithelial cells, has been found to increase adenoid cystic carcinoma scattering and perhaps invasiveness.
4. Expression of proliferating cell nuclear antigen (PCNA) was found in the 2 most common malignant salivary tumors, mucoepidermoid carcinomas and adenoid cystic carcinomas, with higher expression in submandibular gland—derived malignancies.
Classification of salivary gland tumors:
Salivary gland malignant tumors are classified according to their cell types. This classification has been proposed by Seifert and Sobin in 1972. This classification has seven categories:
1. Adenoma
2. Carcinoma
3. Non epithelial tumors
4. Malignant melanomas
5. Secondary tumors
6. Unclassified tumors
7. Tumor like disorders
Histological classification of salivary gland carcinomas:
. Acinic cell carcinoma
. Mucoepidermoid carcinoma
. Adenoid cystic carcinoma
. Polymorphous low grade adenocarcinoma
. Papillary cystadenocarcinoma
. Mucinous adenocarcinoma
. Adenocarcinoma
. Carcinoma ex pleomorphic adenoma
. Malignant mixed tumor
. Squamous cell carcinoma
. Undifferentiated carcinoma
Histological classification is vital in the sense that it makes an attemp to predict survival. For example in the case of adenoid cystic carcinoma it is the histological pattern that is related to survival. It has three distinct histological patterns:
1. Cribriform pattern the most common type
2. Solid pattern
3. Tubular pattern
Among these three types solid pattern has a poor survival rate when compared to the other two varieties.
Acinic cell carcinoma: Is a malignant tumor of low grade malignancy. It commonly involves parotid gland. This is one tumor which can manifest with bilateral involvement. This is second only to warthin's tumor in this regard.
Clinical features: Commonly presents as a painless lump in the parotid region. It is commonly solitary and encapsulated with well defined margins. Multilobulations do occur. This tumor apparently arises from acinar cell. Acinar cell carcinoma has the best prognosis among malignant tumors of salivary glands. Total excision of the mass will ensure cure. Facial nerve can be preserved in these patients, because these tumors are very slow growing ones. Facial nerve is almost never involved in these patients.
Mucoepidermoid carcinoma: Is the most common malignant lesion involving salivary glands. Infact they account for more than one third of cases. It is the most common parotid malignancy. Initially it starts off as painless nodule, and later becomes painful. Facial nerve is invaraibly involved when parotid is affected by this tumor. This tumor is composed of mucous secreting cells, epidermoid cells and intermediate cells. It has been postulated that all salivary gland malignancies arise from a common progenitor cell i.e. the intercalated duct reserve cell.
Histologically mucoepidermoid carcinoma may be classified histologically into low grade and high grade malignancies. Low grade tumors are cystic, where as high grade tumors are solid with areas of necrosis and haemorrhage. Surgical excision of the tumor is the preferred modality of treatment.
Adenoid cystic carcinoma: This tumor commonly involves major salivary glands. Histologically these tumors can be classified into three subtypes:
Solid pattern
Cribriform pattern
Tubular pattern.
Among these subtypes the solid pattern shows the worst prognosis.
These tumors are known for their ability to spread distantly (distant metastasis). They follow the blood borne route and also are known to involve nerves. (Perineural spread is common). Perineural spread has an important relationship with the size of the tumor mass. Greater the size of the tumor higher are the chances of perineural spread. Adenoid cystic carcinoma involving the major salivary glands carry a better prognosis than those involving the minor glands. Perineural spread is common when the tumor involves major salivary glands like the parotid and submandibular. Surgical excision of the affected gland is the preferred modality of management. Post operative radiotherapy is contemplated in patients who show indistinct surgical margins after surgery.
Polymorphous low grade adenocarcinoma: This was previously considered to be the low grade counterpart of adenoid cystic carcinoma. It has a similar histology to that of adenoid cystic carcinoma. Quite recently this tumor has been classified as a separate entity because of its differing behaviour pattern when compared with that of adenoid cystic carcinoma. This type of tumor classically demonstrates four distinct histological patterns:
Tubular
Cribriform
Papillary
Lobular.
These tumors commonly involve female patients, and has a propensity to involve minor salivary glands. Commonly they arise from palatal salivary glands. Surgical excision is the preferred modality of treatment since distant metastasis and lymph node involvment are pretty rare.
Adenocarcinoma / papillary cystadenocarcinoma / mucinous adenocarcinoma: These are the different histological types of a single entity (adenocarcinoma). In fact they can also be considered as variants of adenocarcinoma. Mucinous and papillary cystadenocarcinoma are low grade malignancies. The non mucin secreting variety is the most virulent in this group. Most adenocarcinomas arise from the parotid gland. They constitute only a very small proportion of parotid tumors. They are common in the 6th and 7th decades of life. Females are commonly affected. Surgery appears to be the most favoured treatment modality.
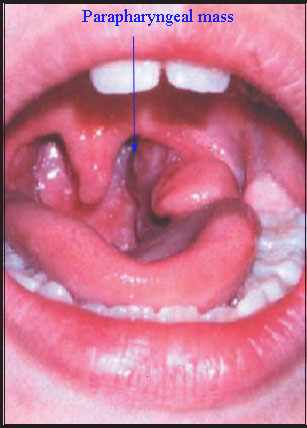
Salivary gland tumor presenting as parapharyngeal mass
Picture showing adenocarcinoma of parotid gland
Carcinoma ex pleomorphic adenoma: These tumors tend to affect major salivary glands They constitute nearly 10% of all malignant tumors involving salivary glands. These tumors arise from pre existing pleomorphic tumors. They are commonly known to involve the deep lobe of parotid gland. Depth of invasion play an important role in the prognosis of this lesion. A depth of invasion of less than 1cm has the best prognosis.
Three different histological types have been described:
1. Non invasive carcinoma
2. Invasive carcinoma
3. Carcinosarcoma
Surgical excision of the mass is preferred.
Squamous cell carcinoma: Primary squamous cell carcinoma involving salivary glands is pretty rare occurrence. Classically these tumors shoud arise from the gland itself and not from the adjoining lymph nodes. There must be no associated tumor in adjoining regions. Surgical excision followed by irradiation is the preferred modality of management.
Undifferentiated carcinoma: These tumors arise from ductal reserve cells. Histologically these tumors are small cell variety. It has been suggested that Ebstein barr virus infection may play an important role in the etiology of these tumors. Irradiation plays an important role in the management of these tumors.
Lymphoma: Batsakis criteria for diagnosis of lymphoma of salivary gland are:
1. Extraglandular lymphoma should not be present
2. Histologically the tumor should involve the glandular parenchyma and not intraglandular lymph nodes
3. Lymphoma markers should be demonstrated by immunohistochemistry.
Lymphomas involving the salivary glands are very rare.
Low grade lymphomas are not treated at all. High grade lesions are managed using chemotherapeutic agents.
Metastatis disease involving the salivary glands: Almost all the major salivary glands are adjacent to lymph nodes. Infact the superfical and deep lobes of parotid glands contain lymph nodes. Almost all of the metastasis of salivary glands arise from the skin of head and neck region. Parotid gland is most commonly involved in these lesions. These tumors are best managed by total resection of the mass followed by block neck dissection.
Malignant tumors of parotid gland:
Statistically speaking one in six parotid tumors are malignant. Tumors involving the superfical lobe of parotid gland enlarges laterally producing swelling just above the angle of the jaw. These tumors lift up the ear lobule. Facial nerve paralysis is common. Pain associated with rapidly enlarging mass is common in malignancy. Carcinomas involving the deep lobe of parotid gland expand medially and could present as lateral pharyngeal mass.
Anatomical difficulties borne in mind before embarking on surgical abalation:
1. Branches of facial nerve seperate the superficial and deep lobes of parotid gland.
2. The proximity of external auditory canal
3. Proximity of carotid vessels
4. Proximity of temporo mandibular joint.
Submandibular gland: 40 % of tumors of submandibular glands are malignant. Adenoid cystic carcinoma is the common malignant tumor seen affecting this gland. Malignant lesions of this gland may involve hypoglossal nerve, followed by trigeminal and facial nerves. Lymph node involvement is also common in these patients.
Surgical abalation is the preferred managment modality in these patients.
Clinical features of salivary gland malignancy:
The following symptoms are ominous:
1. Pain
2. Nerve palsy
3. Skin invasion
4. Enlarged neck nodes
Fine needle aspiration cytology has been the main stay in the diagnosis of salivary gland malignancies.
Accepted treatment modalities of salivary gland tumors:
1. Surgical ablation of the mass
2. Post operative radiotherapy. This reduces loco regional recurrence. This is a must for residual tumors, high grade tumors and tumor specimen with inadequate margins.
Complications of salivary gland malignancy:
1. Nerve palsies: Facial, hypoglossal and lingual nerves can be involved
2. Frey's syndrome
3. Salivary fistulae
4. Nodal metastasis
5. Distant metastasis
