Complications of sinusitis
Anatomically the paranasal sinuses are closely adjacent to vital structures like orbit, brain etc. Complications attributed to sinus infections are caused by spread of infection from the paranasal sinuses to these adjacent areas.
Routes of spread:
1. Bacterial infections from the sinuses can spread through natural dehiscences and weakness of the bony barriers. In chronic infections the surrounding bone undergoes sclerosis, while in acute sinusitis massive osteolysis is commonly seen.
2. Lamina papyracea is a paper thin bone separating the orbit from the ethmoidal sinuses. Congenital dehiscences of this bone is commonly seen through which spread of infection can occur from the ethmoids into the orbit. In childhood the frontal sinuses are underdeveloped and orbital complications are caused commonly by acute ethmoiditis.
3. Floor of the frontal sinuses form the roof of the orbit. In older children and in adults frontal sinus infections can spread into the orbit causing orbital complications.
4. Infraorbital canal in the floor of the orbit is a weak area through which infections from orbit may enter into the maxillary sinus.
5. Spread of infection can also occur via diploic veins present in the frontal bone. These veins are known as the veins of Breschet. This is preceded by thrombophlebitis.
6. Venous connections between the sinuses and the orbit donot have any valves facilitating spread of infection from the sinuses to the orbit.
7. The roots of the second premolar and the first upper molar are intimately related to the floor of the maxillary sinus. This facilitates a two way spread of infection. In cases of isolated maxillary sinusitis dental causes must be suspected.
Predisposing factors responsible for complications:
1. Immunocompromised patient (e.g. HIV)
2. Diabetes mellitus
3. Irregular treatment for sinus infections
4. Inappropriate / Inadequate antibiotic therapy
Orbital complications of sinusitis:
Commonly caused in young individuals. These are frequently due to ethmoiditis. This is the common cause for orbital complication in children. In adults involvement of frontal sinuses could commonly cause orbital complications. In adults acute sphenoiditis can cause involvement of optic nerve leading on to blindness.
Hubert's classification of orbital complications of sinusitis:
Hubert classified orbital complications arising from sinusitis into five groups:
Group I: Inflammatory oedema of eyelids with or without oedema of orbital contents.
Group II: Subperiosteal abscess with oedema of lids or spread of pus to the lids.
Group III: Abscess of orbital tissues
Group IV: Mild to severe orbital cellulitis with phlebitis of ophthamic veins
Group V: Cavernous sinus thrombosis
Smith & Spencer classification of orbital complications:
Group I: Preseptal cellulitis - Characterised by oedema of eyelids without tenderness, visual loss or limitation of ocular mobility.
Group II: Orbital cellulitis without abscess formation - characterised by diffuse oedema of adipose tissues of orbit.
Group III: Orbital cellulitis with subperiosteal abscess formation with displacement of the globe. May or may not be associated with visual loss. Ocular mobility is restricted.
Group IV: Orbital cellulitis with intraperiosteal abscess. Here the displacement of globe is severe with restriction of ocular mobility.
Group V: Cavernous sinus thrombosis.

Clinical photograph of a patient with proptosis due to frontal sinusitis
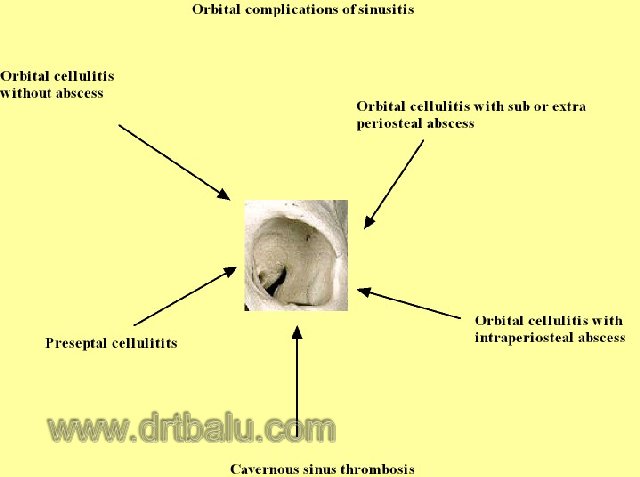
Various orbital complications due to sinusitis
All these ocular complications are associated with pain, tenderness, and displacement of the globe. These symptoms are not seen in preseptal cellulitis. Presence of preseptal cellulitis should be viewed with caution and treated aggressively as it may lead to further sinister complications. If the infection affects the posterior ethmoids and onodi cells optic nerve could be affected. In these patients color vision gets disturbed first. They will have difficulty distinguishing between red from brown and blue from black.
If thrombophlebitis extends posteriorly from the orbit it will involve the cavernous sinus. Opposite side is also affected in this condition. This is one of the common complication of sphenoiditis. These patients will complain of headache, and paraesthesia along the distribution of trigeminal nerve.
All patients with impending complications should undergo a CT scan. This will clearly indicate the site of abscess. Visual acuity tests must be performed. Changes in visual acuity must be distinguished from diplopia due to restricted ocular mobility. Proptosis is always axial in patients with orbital oedema. Severe proptosis will cause chemosis. Sudden increase in proptosis should be relieved within 2 hours if permanent damage to vision is to be prevented. Globe will tolerate even 2cm of displacement if proptosis is chronic as in mucoceles.
These patients must receive broad spectrum antibiotics. These antibiotics must be administered parenterally. If there is any sign of visual disturbance surgical decompression should be immediatly resorted to. Sinus infections must be treated surgically after the acute crisis is over.

Picture showing proptosis due to frontal mucocele
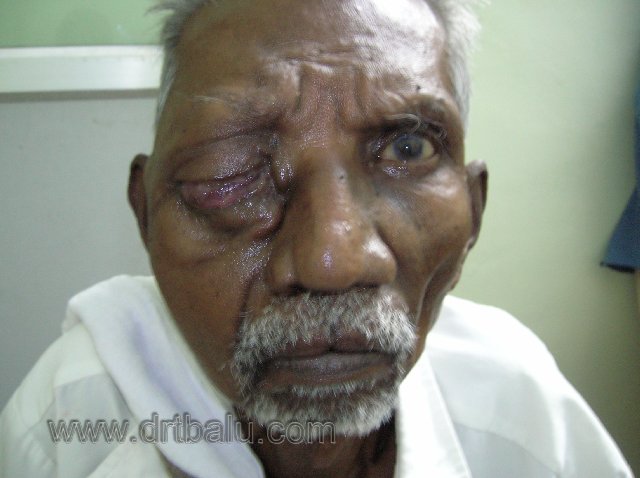
Patient with orbital cellulitis
Long term sequelae of orbital complications:
1. Vision loss
2. Ophthalmoplegia
3. Exposure keratitis due to corneal anesthesia
4. Uveitis
5. Glaucoma
Intracranial complications:
Intracranial complications are less common than orbital complications of sinusitis. These complications can coexist. Intracranial complications are common in adolescents and young adults because the diploic system of veins reaches its peak during adolescence. Males are more commonly affected than females.
Intracrainal complications can be divided into:
1. Abscesses - extradural, subdural or intracerebral
2. Meningitis
3. Encephalitis
4. Cavernous sinus thrombosis, superior sagittal sinus thrombosis
Intracranial abscesses are commonly found subdurally. Second common abscess is frontal lobe abscess. Intracerebral abscess begin as a focus of cerebritis, which gets localised with necrosis and pus formation. Multiple intracranial abscess formation indicates septic thrombophlebitis. These abscesses can be acute or chronic. Abscesses involving the frontal lobe cause very few discomfort or symptoms till a large size is reached. CT scan is diagnostic. Antibiotics must be administered in large doses parenterally to enable adequate concentrations of the drug reaching the brain. Intracranial abscess needs to be drained surgically.
Pott's puffy tumor: is one of the bony complications of frontal sinusitis. This condition was first described by Sir Percival Pott. The frontal bone is a diploic bone with intervening bone marrow. Osteomyelitis of frontal bone leads to this condition. In this condition both the anterior and posterior walls of frontal sinus is involved. Infection may spread anteriorly on to the forehead of posteriorly to form subdural abscess. Debridement of the bone must be performed under cover of intravenous antibiotics.
