Vertigo
Definition:
Vertigo is defined as the subjective sence of imbalance. It has its root in latin word "Vertere" which means to turn. Patient generally has difficulty describing his symptoms.
Synonyms: Vertigo, Dizziness, Unsteadiness.
Types of vertigo: Vertigo can be grossly classified into two types:
1. Rotatory: If the sensation is rotatory it is easy to describe it.
2. Non rotaroty: There is obviously no sence of rotation and the patients have difficulty in describing this sensation.
These groups can further be subdivided into episodic and continuous according to the persistence of symptoms.
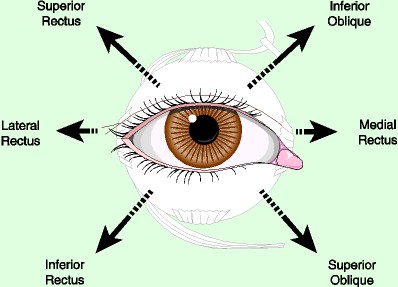
Diagram showing extra ocular muscles that are involved in various ocular movements
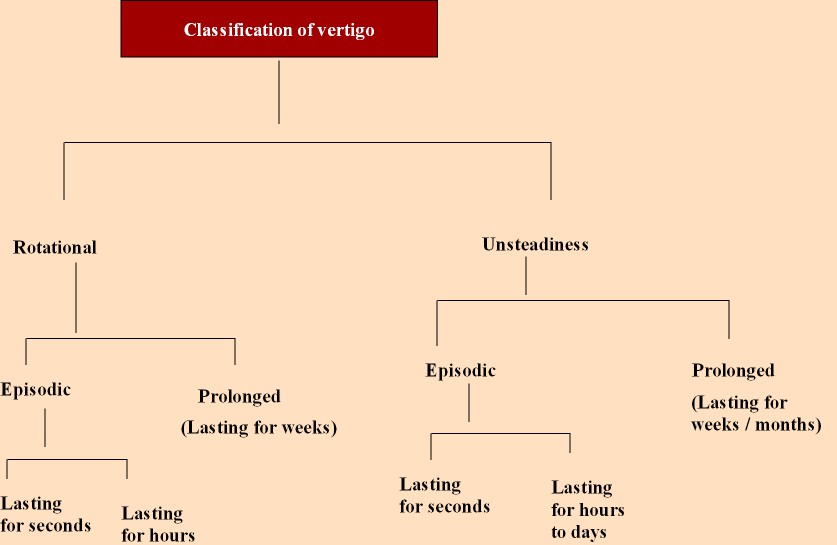
Classification of various types of vertigo
Vertigo can be caused due to disturbances in the inner ear or in the central nervous system. It is important to differentiate the vertigo caused by peripheral and central causes.
Charactersitic |
Central |
Peripheral |
| Severity | Mild | Severe |
| Onset | Gradual | Sudden |
| Duration | Weeks / Months | Seconds / minutes |
| Positional | NO | Yes |
| Fatigable | No | Yes |
| Associted symptoms Assocaited Nystagmus |
Nerologic / Visual Vertical |
Auditory Horizontal |
Table showing features of both central and peripheral vertigo
A detalied history of the disorder is elicited from the patient with specific reference to postural variations, severity, mode of onset etc. The patient must also be quizzed about the associated neurologic / visual / auditory symptoms. Left to themselves the patient may not give the complete story, the examiner will have to take active control of history taking. The patients will be keen to emphasise the aspects which has impressed them the most. The patient should be specifically asked about periods of freedom from vertigo. History taking should be done chronologically.
A detailed history of drug intake is also a must to rule out drug induced dizziness / vertigo. A list of possible drugs are given below:
1. Anti Alzeimers - Drugs used in treatment of Alzeimers disease like memantine, rivastigmine, tacrine can cause dizziness.
2. Anti psychotics - Anti psychotic drugs like chlorpromazine, prochlorperazine, fluphenazine,perphenazine, thioridazine, trifluoperazine can cause dizziness.
3. Antidepressants - Can cause dizziness
4. Anxiolytics - Like diazepam, alprazolam can cause dizziness.
5. Mood stabilisers - Like Gamapentin can cause dizziness
6. Anticonvulsants - Like Phenytoin can cause dizziness
Examination of a Dizzy patient:
As a first step the peripheral causes of vertigo should be ruled out. This can be achieved by a through otological examination. All the cranial nerves must be tested for integrity. Cerebellar function should be assessed by past pointing or by dysdiadokokinesis. Every dizzy patient must be examined for the presence of nystagmus with specific reference to its type. If the nystamus is horizontal then in all probability the cause could be peripheral i.e. auditory. A direction changing horizontal or vertical nystagmus could indicate a central cause for the same.
Examination of corneal reflex: This test is sufficient to test the integrity of the trigeminal nerve. This test is so sensitive that it is positive even in patients with a small acoustic neuromas.
Assessment if facial nerve: can be performed by just looking at the patient when he / she attempts to close the eyes. They will have inability to bury their eyelashes during tight closure of eyelids.
Performing a routine audiogram will assess 8th nerve function.
Cranial nerves 9th and 10th can be rapidly tested by looking for gag reflex. 11th nerve can be tested by asking the patient to shrug the shoulders, which is not possible if the nerve is affected. Hypoglossal nerve can be assessed by just asking the patient to protrude the tongue. It always tends to deviate towards the side of paralysis, inaddition there may be wasting of tongue musculature on the side of the lesion.
Blood flow through the carotids should also be carefully examined to rule out carotid occlusion as a cause of giddiness. Patient's blood pressure and blood sugar levels must also be measured.
Nystagmus:
Presence of Nystagmus along with vertigo is always organic. Nystagmus is defined as a disturbance in ocular posture, characterised by a more or less rhythmical oscillation of the eye ball. The speed of the ocular movements may be the same in both directions or may be quicker in one directior when compared to the other. The direction of nystagmus is also important, a vertical nystagmus is more common in central causes of vertigo.
Basics of ocular movements: The movement of eyeball is controlled by 6 extraocular muscles i.e. 4 rectus and 2 oblique muscles. Among these muscles the superior oblique muscle is innervated by trochlear nerve, and lateral rectus by abducens nerve. All the other muscles are innervated by oculomotor nerves. There is something unique in the oculomotor supply, i.e. it innervates the ipsilateral ocular muscles except for superior rectus which receives it supply from the contralateral side.
The superior oblique muscles are supplied by the contralateral trochlear nerve. The abducens nerve have two types of neurons:
1. Motor neurons innervating the ipsilateral lateral rectus muscle
2. Internuclear neurons supplying the contralateral medial rectus muscle.
Axes and planes of ocular movements: The axes and plane of ocular movements should be clearly defined before an assessment could be made. Three axes have been referred:
1. X axis : Also known as parasagittal or naso occipital
2. Y axis : Also known as transverse or interaural
3. Z axis : Also known as vertical axis
Movement along these axis are described as:
Torsional - Roll or rotation about X axis.
Vertical - Pitch or rotation about Y axis
Horizontal - Yaw or rotation about Z axis
Primary position of the eye: is the postion of the eye in which there is pure horizontal or vertical rotation is associated with zero torsion. Clinically this position refers to the position of the eye when looking straight ahead with the body and head held straight and erect.
Secondary position of the eye: is reached by pure horizontal or vertical rotation of the eye.
Tertiary position of the eye: is reached when there is a combination of horizontal and vertical rotation from the primary position
Torsional eye movements: These are rotatory movements of the eye ball. When the eye ball rotates in such a way that the upper pole of the eye tilts towards the right of the subject it is known as clock wise rotation (always in the subject's point of view). When the upper pole of the eye tilts towards the left of the subject it is known as counter clock rotation.
The position of the eye ball is dependent on two sets of impulses, the visual and vestibular. The visual impulses are concerned with maintenance of position of eye in relation to the object of interest. The vestibular impulses help in maintainance of the position of eye ball in relation to that of the head.
Pendular nystagmus: is a horizontal to and fro movement of the eye ball. The to and fro movements are almost equal in velocity. This is commonly seen in patients with blindness. The eye ball is attempting to focus the image at the fovea of the retina. Since the patient is blind the eye ball keeps searching for visual object to focus hence this nystagmus. It is also known as the Blind Man's nystagmus.
Horizontal nystagmus: This is characterised by rhythmic oscillations in which the movement in one direction is significantly faster than the other. The slow movement is the pathological one while the faster one is the corrective component. The direction of the corrective faster movement is used to denote the direction of the nystagmus. The position in which the nystagmus is least marked is known as the Null point.
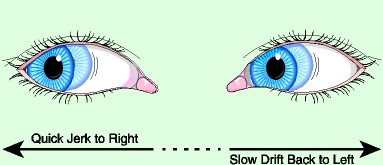
Figure showing horizontal nystagmus
Spontaneous nystagmus: is said to occur when the rhythmic movements are present on the forward gaze.
Induced nystagmus: is said to occur when the rhythmic movements of the eye are brought about by some specific test.
Gaze nystagmus: or intermediate nystagmus is said to occur during extremes of lateral or vertical gaze positions.
Procedure for examining for nystagmus:
1. The patient should be positioned in good light.
2. The object of focus should be at infinity
3. While looking for lateral gaze nystagmus care must be taken to ensure that the nose does not block the field of vision.
Causes for spontaneous nystagmus:
Labyrinthine: Labyrinthine nystagmus is usually biphasic. Its features are:
a. It is usually associated with a sensation of vertigo
b. It is always unidirectional.
c. It is more marked when looking at the direction of the fast phase
d. It is enhanced on removal of optic fixation or on eye closure. Frenzels glasses can be used to remove optic fixation. It is actually a 10 diopter glasses worn by the patient. It removes optic fixation there by enhancing labyrinthine nystagmus. These glasses makes the eye look larger when viewed by the observer. Even small degrees of nystagmus will be noticed.
e. The nystagmus produced is fatiguable
Central nervous system lesions causing spontaneous nystagmus: Nystagmus caused by lesions involving the central nervous system has the following features:
a. Nystagmus is bidirectional (direction changing)
b. Nystagmus could be commonly vertical
c. Nystagmus usually is non fatiguing in nature
d. Nystagmus is not enhanced on removal of optic fixation
Nystagmus caused due to drugs and toxins:
Drugs and toxins cause nystagmus by their effect on the central nervous system. The nystagmus induced by toxins and drugs more or less resembles that of central nervous system nystagmus
Ocular nystagmus: Any lesion affecting the macula, especially when the peripheral vision is still maintained may cause nystagmus which is pendular in nature. This nystagmus commonly occur in ambylopia. Miner's nystagmus also fall into this category.
Congenital nystagmus: is often familial, usually horizontal and pendular. The null point in this type of nystagmus is close to the position of forward gaze. Closure of the eyes results in reduction of nystagmus.
Causes of induced nystagmus:
Nystagmus may be induced by clinical testing or by certain investigations. The most common clinical test inducing nystagmus is the positional test (Dix Hallpike manoeuver). This is useful in diagnosing BPPV. This procedure is explained in detail under the topic BPPV.
Another way of inducing nystagmus is by performing a fistula test. This test is positive in the presence of labyrinthine fistula. In this test nystagmus and giddiness is induced by altering the pressure of air in the external canal.
Exposure to loud sounds in these patients also can cause nystagmus and giddiness. This is known as Tullio phenomenon.
In clinical setting nystagmus can be induced by performing caloric tests / cold caloric tests or by the use of optokinetic drum which can stimualte optokinetic nystagmus.
Oscillopsia: is the term used to describe the illusion of motion of environment due to an inadequate vestibulo ocular reflex. During head and body movements images are held steady on the retina by the presence of vestibulo ocular reflex. Patients with reduced peripheral vestibular function often have oscillopsia. One method for testing for oscillopsia is to test the patients visual acuity with a Snellen eye chart with the head held still, and repeating the same test during passive high frequency head movements produced by the examiner. The patient will have reduction in acuity if oscillopsia is present.
Investigations:
1. Audiometry
2. Caloric tests
3. Electric nystagmography
4. CT scan / MRI scan to rule out acoustic neuromas / CNS lesions
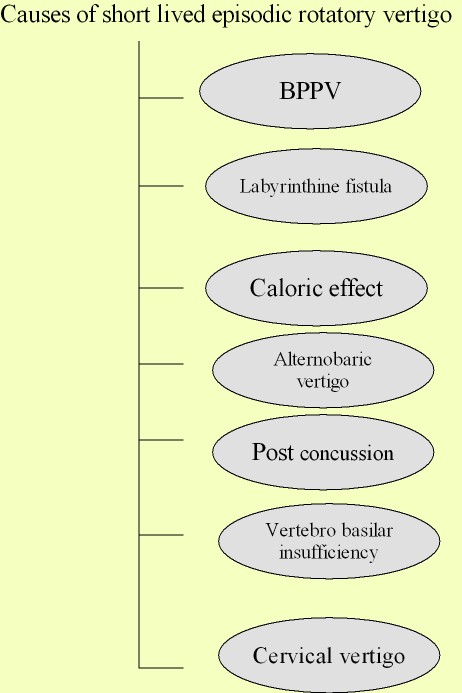
Figure showing various causes of vertigo
Alternobaric vertigo is caused due to sudden change in altitude. This occurs in fighter pilots due to sudden altitude changes which occur during flying military jet fighter planes.
Episodic vertigo can also occur due to metabolic failure of labyrinth as seen in:
1. Menier's disease
2. Syphilitic labyrinthitis
3. Delayed endolymphatic hydrops
4. Following middle ear surgery.
Destructive lesions of labyrinth: Can cause prolonged rotatory vertigo lasting for more than 24 hours, usually less than 3-4 weeks. These include:
1. Vestibular neuronitis
2. Trauma: Head injury, Ear surgery, Labyrinthectomy, and vestibular neurectomy
3. Labyrinthitis: Bacterial / viral
4. Vascular lesions
5. Metastatic deposits in CP angle
Unsteadiness: Patients who are unsteady may have problems describing their symptoms. Commonly it could be due to:
Physiological overload: Unsteadiness caused due to physiological overload of the vestibule or the central processing systems may cause unsteadiness. This could occur due to:
a. Excessive input as can happen in a normal person with very rapid movements.
b. May also occur as a result of abnormal input, especially from visual apparatus
c. It may result from minor inadequacies in visual, proprioceptive or labyrinthine systems.
Unsteadiness lasting for hours / days may be due to temporary impairment of central vestibular connections or decompensation of vestibular system. Drugs are the most common cause for this temporary unsteadiness. Other causes include travels sickness, perilymph fistula, Active chronic suppurative otitis media, hyperventilation.
Vestibular inadequacy may cause unsteadiness lasting for weeks or months. This is often seen in elderly. Vestibulo toxic drugs like gentamycin can cause unsteadiness.
Vertigo following head injury may be due to:
a. Post concussional syndrome
b. BPPV
c. Perilymph fistula
d. Delayed hydrops
Treatment of vertigo:
Vestibular system can be suppressed by using labyrinthine sedatives like cinnarazine.
Wait for compensation to occur: In all peripheral causes of vertigo central compensation eventually occur in 6 weeks time. Patient should be encouraged to performed labyrinthine exercises.
As a last resort the offending labyrinth can be eliminated by using intra tympanic drugs like streptomycin or surgical labyrinthectomy.
